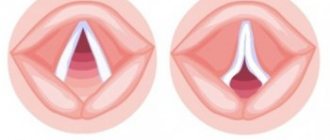
False croup or acute obstructive laryngitis is an emergency pathology that affects the upper respiratory tract. False croup is based on a sharp narrowing of the lumen of the larynx: breathing is impaired, a “barking” cough and hoarseness appear. False croup affects children from 6 months to 6 years. This is due to the anatomy and physiology of the respiratory tract: in children, the diameter of the vestibule and the funnel-shaped shape of the larynx are small, the vocal folds are short and located high. These structural features contribute to the development of the croup.
In children of different ages, the prevalence of croup varies: more than 50% of patients are children from 2 to 3 years old, children aged from 6 to 12 months are less common. Children over 5 years of age almost never get false croup.
What causes false croup?
Acute obstructive laryngitis develops due to a viral infection. 80% of croup cases are the result of the parainfluenza virus. The remaining 20% is influenza A and B virus, respiratory syncytial virus, enterovirus, adenovirus, rhinovirus or coronavirus.
The following factors increase your risk of developing croup:
- immaturity of reflexogenic zones;
- predominance of the parasympathetic nervous system;
- soft and pliable cartilaginous skeleton;
- congenital anomalies of the respiratory tract.
Predisposing factors also include: allergies to medications, damage to the central nervous system during childbirth, prematurity, overweight of the child and allergies in parents.
The source of infection is a sick person who transmits viruses or bacteria through coughing and sneezing. The incubation period is from 7 to 10 days. The incidence of false croup depends on the season: the risk of infection increases in autumn and winter.
Causes
There are many reasons for the development of this disease in children, but most often this disease develops as a result of a viral or bacterial infection that affects the respiratory tract. These can be viruses that cause diseases such as influenza, parainfluenza, RS virus, adenoviruses. As for bacterial damage to the respiratory tract, they can be Haemophilus influenzae, staphylococci, pneumococci, as well as some types of streptococci.
Reasons why false croup occurs in childhood:
- due to the functional immaturity of some reflexogenic zones, in this case the parasympathetic nervous system predominates;
- with a small cartilage diameter;
- if the cartilage is loose and pliable;
- with a high position of the vocal cords and if they are short;
- funnel-shaped larynx;
- narrow lumen of the larynx;
- if the muscles that are located around the glottis are hyperexcitable;
- if there are many vessels in the mucous membrane, but at the same time there are not enough elastic fibers.
In addition, there are a number of features that increase the likelihood of the disease occurring. For example, this could be a birth injury, paratrophy or allergic reactions. Children born by caesarean section are also susceptible to this disease. Naturally, the likelihood of illness increases if the child constantly suffers from colds, as well as during the period when a vaccination was recently given.
This disease occurs due to the fact that the virus that enters the respiratory tract does not immediately leave the body, but begins to multiply, and accordingly, the inflammatory process starts. Because of this, as with any inflammation, swelling appears and excess mucus is formed. Due to swelling, the affected organs enlarge, which leads to a narrowing of the glottis. This explains why there is a problem with the voice and difficulty breathing.
Symptoms of false croup
False croup begins with nonspecific symptoms. In the first three days after the onset of the illness, the child develops a cough and runny nose, and the body temperature rises to 37–39 0C. The child is agitated, sleeps poorly, cries, refuses toys and does not want to eat.
Signs of the disease begin 3 days after the incubation period. Symptoms usually worsen in the evening or at night. The child suddenly wakes up with a “barking” and rough cough. Noisy and labored breathing appears, as if the child is not getting enough air. The child gets scared, begins to worry and cry. This condition lasts another 1–2 days.
Symptoms are caused by gradual inflammatory swelling in the subglottic region of the larynx. The vocal cords leak out with a cellular infiltrate, and thick mucus accumulates on the walls of the airways.
At this stage, the main symptoms of false croup appear:
- hoarseness (dysphonia);
- difficulty breathing;
- “barking”, jerky and short dry cough.
Inspiratory stridor joins the clinical picture. This is wheezing, which occurs due to the fact that air quickly passes through the narrowed lumen of the larynx.
When it becomes difficult for a child to breathe, the auxiliary respiratory muscles of the chest are activated, and the supraclavicular and jugular fossae are retracted. Outwardly, it becomes noticeable how the child’s nose wings expand to inhale more air.
Due to lack of oxygen in the blood, other symptoms appear. The child becomes lethargic or agitated. The skin becomes pale and the area around the mouth turns blue.
How does false croup occur?
The disease progresses differently in children. The severity of false croup is determined by four degrees:
- First degree of severity. The child periodically gets excited or becomes lethargic, but clarity of consciousness remains. Swollen wings of the nose are visible, breathing is not rapid. There is slight hoarseness and a “barking” cough. With little physical activity, breathing becomes noisy. The first degree lasts from 2–3 hours to 1–2 days.
- Second degree. Consciousness is clear, but the child is in constant agitation: he cries, screams, cannot sit still, does not sleep. When breathing, the intercostal spaces are retracted. Breathing and pulse are slightly increased. In a state of calm, the child breathes loudly. The face is pale. The second degree lasts up to 3–5 days.
- Third degree. Consciousness is confused: the child is disoriented, lethargic and drowsy, may not recognize his relatives and may not understand where he is. All auxiliary muscles of the chest are included in the respiratory act. Breathing is shallow. The voice has shrunk. The cough is rough and loud.
- Fourth degree of severity. This is a state of asphyxia when almost no oxygen reaches the lungs. The child is unconscious, the auxiliary muscles are almost not involved in the respiratory act. The breathing itself is intermittent and inconsistent. The pulse is hard to palpate. Seizures may occur due to a serious disturbance in the blood gas composition.
Acute obstructive laryngitis can be complicated by bacterial tracheitis, purulent laryngotracheobronchitis and pneumonia. In the most severe cases, death occurs.
If you notice a specific triad of symptoms (hoarseness, barking cough and difficulty breathing) and signs of an acute respiratory viral infection (fever, runny nose, drowsiness or restlessness in a child), call an ambulance.
For diagnosis, doctors collect medical history, complaints and information about vaccination. The doctor examines the child, measures body temperature, records the number of respiratory acts and heart rate. Afterwards, laboratory and instrumental methods are prescribed: general blood test, biochemical blood test, radiography, virological diagnostics, bacteriological examination. To clarify the diagnosis, the doctor invites an ENT specialist for a consultation and prescribes fibroendoscopy of the larynx.
The parent can call a doctor at home. In this case, the doctor conducts a rapid diagnosis: assesses the voice, the presence of a “barking cough”, looks at the child’s breathing, and clarifies how long ago the signs of an acute respiratory viral infection appeared. To objectively assess the child’s condition, the doctor assesses the patient’s severity using the Westley scale. This scale includes the following indicators: wheezing noisy breathing, blue skin tone, degree of consciousness, breathing and retraction of auxiliary muscles in the respiratory act.
If the child is objectively at grade 2, 3 or 4, urgent hospitalization is indicated. The latter is also indicated in the following cases:
- child is less than 1 year old;
- the medications had no effect;
- the child was born premature;
- the patient has a concomitant disease or congenital malformations.
If you see that the child has a second or more severe degree, there are indications for hospitalization, call an ambulance or get to the hospital on your own.
Treatment of Croup
Mild cases
In most cases, laryngitis and false croup can be effectively treated at home. Doctors and nurses can easily monitor a child's progress by talking with parents over the phone and advising them on first aid for croup. Cold humidification will help your baby breathe easier while he sleeps. Painkillers will help ease the discomfort. Preparations for croup cough should be prescribed only after consultation with a doctor.
Severe cases
If your child has trouble breathing, you should go to a hospital or clinic. Doctors may prescribe steroid medications to open your child's airways to make breathing easier. They may be prescribed for use at home. In extreme cases, using a breathing tube may help your child get enough oxygen. If a bacterial infection is determined to be responsible for the croup, antibiotics will need to be taken while in the hospital. If the patient is dehydrated, intravenous fluids may be required.
Treatment of false croup in children
The doctor’s task is to restore breathing as quickly as possible, improve the child’s general condition and prevent the progression of laryngeal stenosis. To do this, the doctor prescribes glucocorticosteroids, which block inflammation, relieve local swelling and reduce the permeability of the vascular walls.
When providing emergency care, a string or membrane nebulizer is used, which contains a glucocorticosteroid - budesonide. This substance quickly enters the respiratory tract and has a strong local anti-inflammatory and vasoconstrictor effect. The effect occurs 15–30 minutes after administration of the medicine. The sustained effect of budesonide occurs within 3–6 hours. If budesonide is not available, the emergency medical team uses epinephrine, an adrenal hormone.
In hospital conditions, systemic glucocorticosteroids - dexamethasone or prednisolone - are used to treat acute obstructive laryngitis. To stabilize the condition, medications are administered for another 2–3 days. When the child gets better, the doctor reduces the dose.
Other means are used to treat false croup:
- antiviral: they are prescribed if the doctor knows that false croup is of viral origin. Neuraminidase inhibitors have proven clinical effectiveness in stopping the influenza virus. The greatest effect of antiviral drugs is observed in the first 48 hours after the onset of the disease;
- antibacterial agents: prescribed if there are laboratory signs of bacterial origin. In addition, they are given to the child if complications of a bacterial nature are observed;
- if there is obstruction of the lower respiratory tract, the doctor prescribes bronchodilators, for example, Berodual or salbutamol;
- when the acute period of the disease has passed, the doctor prescribes mucolytics - medications that thin the sputum. Medicines are administered by inhalation or orally.
The doctor observes the little patient for several days. Treatment is considered effective in the following cases: the larynx allows air to pass through and the child breathes freely, body temperature is normal, and there are no bacterial complications. If the criteria are met, the child is discharged from the hospital.
What to do after leaving the hospital:
- the next day after discharge, you need to call your local doctor to examine the child;
- continue symptomatic treatment of acute respiratory viral infection;
- Vaccinate your child against influenza within two weeks after complete recovery (if vaccinations have not been done before).
Parents should forget about traditional medicine when their child has acute obstructive stenosis. While ineffective and untested “grandmother’s” treatment methods are used, swelling of the larynx increases and it becomes increasingly difficult for the child to breathe.
While parents are waiting for the ambulance, you need to calm the child down and use a distraction therapy method - put a warm compress on the neck with Vaseline oil. The essence of the method is that heat has a local effect on soft tissues: the neck muscles relax and it becomes easier for the child to breathe. It should be remembered that this will only give a temporary effect and cannot replace full treatment with a warm compress. The use of steam inhalation is not recommended. They are excluded from international protocols for the treatment of croup.
Symptoms of false croup that should prompt immediate medical attention
Questions that parents often have are what false croup is in children, the symptoms and treatment of this disease, how dangerous it is for the child and whether it will cause irreversible processes in the small body. The first thing you need to know is that this disease is quite serious, and if left untreated, it can lead to dangerous consequences for the baby’s health. That is why it is so important to start treatment as early as possible - the chances of a successful recovery increase several times.
Symptoms of the disease that parents should pay attention to:
- night coughing attacks accompanied by shortness of breath, difficulty breathing;
- sputum is practically not coughed up, which often leads to injuries to the respiratory tract; blood may be seen in the scanty mucus released;
- hoarseness of voice appears;
- often coughing attacks turn into severe vomiting;
- the child’s skin turns pale, fingertips and lips acquire a threatening blue tint;
- temperature rises;
- The baby is bothered by a runny nose and severe sore throat.
Already the first signs of the disease should be a reason to go to the doctor - it is strictly not recommended to start treatment on your own.
How to prevent false croup in a child?
To prevent false croup in a child, you need to adhere to the following measures:
- vaccinate against influenza every year;
- increase the child’s overall resistance to infections with proper nutrition and good sleep;
- prevent infections by constantly and thoroughly washing your hands, ventilating the room with cool and moist air, and drinking plenty of fluids.
Some prevention methods need to remain in history. For example, prevention with vitamin C, herbal remedies and homeopathic medicines has no proven effectiveness.