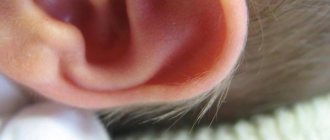
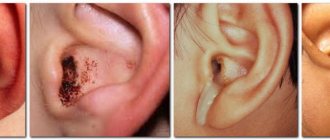
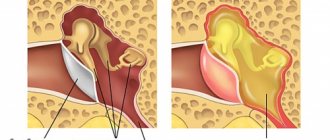
General information
The presence of exudate in the ear of a child or adult always indicates the development of pathological processes. Moreover, they can occur not only in the hearing aid, but also in the upper parts of the respiratory system, since they are interconnected with each other. The discharge itself can be different:
- bloody;
- purulent;
- cloudy;
- transparent;
- brown;
- white;
- black;
- yellow (orange).
The consistency of the released exudate can be liquid, like water, viscous, or thick, like cottage cheese. There may be no specific odor, but, as a rule, in the presence of purulent and inflammatory processes it is present.
Sometimes people secrete a yellow liquid, which many perceive as a pathology. But 80% is ordinary sulfur with a liquid consistency. It does not have an unpleasant odor and its presence does not cause other symptoms characteristic of pathologies (hearing loss, pain, etc.) in a person.
But in order to understand that the discharge of fluid is natural and does not indicate the presence of any disease, it is necessary to consult a doctor, since some pathologies can be asymptomatic for a long time and the presence of abundant sulfur may be the only sign of their development.
As a rule, pathological fluid begins to be released from the ear due to infection or inflammation. Allergic reactions and mechanical damage to the hearing aid can also provoke its occurrence. Only a doctor can determine the exact reason why fluid flows from the ear, taking into account the nature of the exudate, medical history and examination.
Antibiotics for treating ears: list
If it flows from the ear, then patients with purulent otitis are prescribed:
- Flemoclav. This is a combination medicine that consists of two active ingredients: clavunatic acid and flemoxin. The acid enhances the effect of the antibiotic and contributes to its higher effectiveness.
- Augmentin. A broad-spectrum drug that is prescribed for complications of ARVI. Effective against most diseases of the hearing, nose and throat organs.
- Amoxicillin. This is a broad-spectrum penicillin. It is also prescribed for ailments of the ENT organs.
In order to cope with the pathology, it is necessary to react in time to the appearance of painful sensations and consult a specialist. In addition, you should take care of yourself, avoid drafts, as well as getting foreign objects or liquids into your hearing organs. To perform hygiene procedures, you do not need to use cotton swabs, paper clips or matches. It is enough to moisten the turunda in alcohol or a solution of hydrogen peroxide, and clean the ear canals without deep immersion.
Pus from the ear
Symptoms
The development of pathological processes in the hearing aid can be manifested not only by the release of exudate, but also by a number of other symptoms. For example:
- Decreased hearing quality.
- Headaches.
- Sensation of a foreign body in the ear.
- Redness of the skin lining the inner surface of the outer ear.
- Weakness.
- Dizziness, etc.
With the development of acute otitis, the patient may be bothered by throbbing pain in the ear canal, purulent discharge, fever, migraines, etc. In children, it is often accompanied by signs of ARVI - fever, cough, nasal congestion, etc. As soon as the hearing aid is released from purulent contents, the condition is normalized.
Important! Chronic otitis media can be asymptomatic for a long time. The above-described signs of the disease occur only during its exacerbation and require immediate treatment.
The occurrence of mastoiditis often manifests itself:
- Headache.
- Swelling and redness of the skin behind the ear.
- Release of stretchy fluid.
- Fever.
If no therapeutic measures are taken in the initial stages of mastoiditis, this can lead to serious consequences. The thing is that this disease often causes complications in the brain and leads to the destruction of its cells.
When bacterial dermatitis appears, patients often complain that their ear hurts, the skin behind it swells and turns red, and crusts form in the ear canal itself, which are difficult to separate.
Black exudate often occurs during the development of cancer. As a rule, it is accompanied by severe headaches and discomfort in the ear canals, which is caused by the pressure of the tumor on nearby tissues and nerve endings.
Discharge from the ear (Otorrhea): diagnosis and treatment
What is the nature of the discharge?
Ear discharge can be classified according to its sources
- Outer ear
- Middle ear/mastoid
- Inner ear
Below are the conditions associated with each of these sources, each of which may be accompanied by ear discharge. More than one disease may be present, for example chronic otitis media can lead to otitis externa.
The most common conditions encountered in daily clinical practice are highlighted in bold italics. For this reason, these conditions will receive more attention.
| Outer ear | Otitis externa; Polyps/granulation tissue; Boils; Foreign body; Cholesteatoma of the external ear/keratitis obturans; Malignant otitis externa; Injury; Carcinoma |
| Middle ear | Acute suppurative otitis media Chronic suppurative otitis media - mucous chronic suppurative otitis media - cholesteatoma Polyps/granulation tissue; Leakage of cerebrospinal fluid; Carcinoma |
| Inner ear | Leakage of cerebrospinal fluid |
How can I tell what the origin of ear discharge is?
A thorough history is vital.
Anamnesis
Age
Ear discharge in children is more likely to result from otitis media than from otitis externa. In the case of ear discharge in adults, the opposite situation occurs.
Duration of ear discharge
A short history of ear discharge is more common with acute infection
History of foreign body/middle ear ventilation tube
A history of a middle ear ventilator tube or a foreign body in the middle ear may cause infection.
History of head injuries
A history of head trauma indicates the possibility of a basal skull fracture or cerebrospinal fluid (CSF) leak.
Immunosuppression
It is an important factor in the development of malignant otitis externa. Reduced immunity in children may be a factor in the recurrence of ear, nose and throat infections.
Survey
Mastoid
Sensitivity of the mastoid process may be due to pathology of the mastoid process or due to inflammation of the retroauricular lymph nodes.
Outer ear
Pay attention to the color, texture and presence of any inflammation. Pay attention to scars from previous surgeries. Examine the outer ear by palpation to assess temperature and tenderness.
auditory canal
Is the ear canal congested or inflamed? Can you see a foreign body or polyp?
Discharge
Is there mucus, blood, clear fluid (CSF), pus, or keratin (cholesteatoma) in the ear canal? The middle ear has a large number of mucus glands, so if the discharge is mucous, it must be from the middle ear. Blood may appear in ear discharge due to injury or carcinoma.
Eardrum
Can you see her? If not, why not? Is it due to excessive ear discharge, complex anatomy, or an uncooperative patient? You must be able to see the eardrum to confirm the diagnosis.
What are the principles for diagnosing the disease?
Most diagnoses are obvious with a careful history and careful examination of the inside of the ear. Taking samples of ear discharge is necessary for testing, which can identify pathogens that are more common in this location than in others (see otitis externa and otitis media). The use of careful examination with a microscope is useful, especially if microaspiration is necessary: however, this often requires referral to the local ENT department.
Otitis externa
Etiology
Most cases of otitis externa are associated with Pseudomonas aeruginosa or staphylococcal infection. Other bacteria, viruses and fungi can play the role of pathogen.
Symptoms
Pain, irritation and discharge from the ear with an unpleasant odor. Occasionally, a history of cotton swab use, swimming, and/or diabetes may be causes of otitis externa.
Signs
Edema, narrowed ear canal with exudate and detritus. In acute otitis externa, patients may often have concomitant inflammation of the tympanic membrane, as the tympanic membrane may also be involved. The appearance of the eardrum with external chronic otitis may not have any features. Patients rarely feel unwell. Posterior auricular lymph nodes can often be palpated and may be tender. These signs may be confused with mastoid tenderness in conditions such as mastoiditis. Differential diagnosis with mastoiditis is carried out by examining the ear. Patients with mastoiditis often have no symptoms related to the outer ear, but they may have middle ear effusion and tend to be young. Sensitivity of the cartilage of the auditory canal upon palpation of the auricle is a sign of external otitis.
Other causes of otitis externa may be considered. Boils caused by staph infection can cause localized otitis externa and contribute to the development of an abscess. A vesicular rash on the pinna and/or external auditory canal may be a sign of a viral infection (varicella). This may be accompanied by facial palsy and sensory hearing loss in Ramsay Hunt syndrome (tinea ear).
Treatment
Acute external otitis: The key to effective treatment is careful cleansing of debris from the ear canal and local application of antibiotic drops. Ear cleaning must be repeated constantly. It may be necessary to insert ear packs containing antibiotic drops if the ear canal is too narrowed by swelling to use drops. Antibiotic drops containing steroids often help reduce swelling in the ear canal. Strong pain relief may be necessary.
Chronic otitis externa: Chronic otitis externa should raise suspicion for an atypical pathogen such as a fungus. This is confirmed by the results of swab tests from the ear canal, and treatment consists of the use of antifungal drugs. Applications of antifungal drugs should continue for at least one month. Often the clinical picture does not appear for a long time while the fungal spores are in a latent state, until the external auditory canal is repopulated.
Chronic otitis externa, especially in people with reduced immunity, can cause the development of malignant otitis externa (see below). Unfortunately, there remains a group of patients with a chronic inflammatory process that affects the soft tissues of the external auditory canal. These patients require repeated treatment with a variety of topical medications. Some patients may benefit from allergy testing or referral to a dermatologist. In cases of medial stenosis due to otitis externa, or if there is a possibility of chronic infection of the soft tissue or bone, surgery may be required. Topical ear drops may worsen otitis externa, especially if there is an allergic sensitivity to the drops being used or if the otitis externa is due to dermatitis or psoriasis.
Prevention
Medicines such as EarCalm and preventative measures to keep water out of the ears can reduce the incidence of otitis externa (otitis externa is more common in swimmers). Efforts to improve personal hygiene are helpful, as is avoidance of cleaning the ear canal with fingers or other objects. Topical steroids may be considered as a prophylactic measure if patients have associated dermatitis.
Acute purulent otitis media
Etiologically significant pathogens
In 65-70% of cases there may be positive bacterial culture results. Pathogens characteristic of the respiratory tract are usually identified: Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis. Respiratory viruses are present in 40% of patients with nasopharyngeal discharge at the time of diagnosis of acute suppurative otitis media.
Symptoms
Fever, pain and hearing loss before ear discharge begins. Resolution of pain symptoms with the appearance of ear discharge. It is often associated with or develops after a concomitant upper respiratory tract infection.
Signs
Perforated eardrum with purulent contents in the middle and outer ear. Perforation of the eardrum may not be visible due to the presence of purulent contents in the ear canal.
Treatment
The initial stages of acute suppurative otitis media are not associated with ear discharge. Often, when the eardrum is perforated and fluid is released from the middle ear, there is no risk of further complications and no further treatment is necessary. It was demonstrated that 60% of children with acute suppurative otitis media had improvement after 24 hours, and 81% recovered without drug treatment. Antibiotics may have the effect of reducing the time it takes for pain to disappear. The estimated number of patients required to treat was 1/0.14. Buchem et al. (1981 and 1985) proposed a strategy that recommended keeping antibiotics in reserve for those children who did not improve after 24 to 48 hours.
Prevention
The incidence of acute otitis media can be reduced by using low prophylactic doses of antibiotics. However, concerns about the development of tolerance to antibiotics have limited their clinical use. Placement of a middle ear ventilation tube is sometimes necessary, which also prevents further cases of otitis media while the tube is in the ear canal.
Chronic suppurative otitis media
Chronic Suppurative Otitis Media - Mucous
Mucous Chronic Suppurative Otitis Media is a clinical condition where the ear continually leaks discharge through a perforation of the eardrum or a ventilation tube. Mucous chronic purulent otitis media must be distinguished from chronic purulent otitis media, which refers to cholesteatoma. Currently, otologists view mucous chronic suppurative otitis media as a result of chronic secretory otitis media rather than acute otitis media, which is accompanied by discharge. Some studies have shown that 50% of patients with a ventilator tube will develop at least one episode of ear discharge, and up to 3% will have chronic ear discharge lasting more than six weeks.
Symptoms
Chronic ear discharge that is usually clear or mucous but may be infected (purulent). There may be a history of trauma, placement of a ventilation tube, or perforation of the eardrum associated with otitis media.
Signs
A perforated eardrum may be accompanied by infection, mucus, or be completely dry and clear. Granulation may be visible in the lumen of the middle ear. Fever, pain, or dizziness should raise suspicion of complications.
Chronic purulent otitis media - cholesteatoma
Classic cholesteatoma
Classic cholesteatoma with purulent discharge
Cholesteatoma refers to the presence of skin in the middle ear. The exact cause of this phenomenon is unknown. Cholesteatoma can be acquired (migrating from the eardrum) or congenital (present from birth with an intact eardrum in the middle ear).
Symptoms
Foul-smelling ear discharge, hearing loss and tinnitus. Complications may include dizziness and/or facial paralysis. Rarely, this can lead to intracranial infections (meningitis, brain abscess).
Signs
Keratin residues of a mass with an unpleasant odor in the ear canal. There is often a need to clean the ear to fully determine the size of the cholesteatoma, and this requires contacting an ENT doctor. Cholesteatoma may be visible or may be hidden by a retracted pouch associated with retraction of a segment of the tympanic membrane. Conductive hearing loss is possible. Serious illness can be caused by anything from mild conductive hearing loss to profound sensorineural hearing loss.
Treatment
Patients require appropriate examination to determine the extent of the disease. This requires adequate visualization of the ear using an operating microscope; Sometimes general anesthesia in young children may be necessary to adequately examine and clear the ear of residual debris. The definitive treatment is surgery. However, frequent ear cleaning and the application of local antibiotics at regular intervals or continuously in patients who are not subject to surgery play an important role.
Malignant otitis externa
Malignant otitis externa is not a neoplastic condition, but it is a form of necrotizing external otitis that results in osteomyelitis of the temporal bone and multiple cranial nerve palsies. The exact term used to define this condition is controversial because... the word "malignant" is misleading. It is probably better to describe this condition as otogenic osteomyelitis of the skull base.
Symptoms
Chronic severe pain, especially at night. Patients often have diabetes or a weakened immune system, or are advanced in age.
Signs
Granulation tissue on the lower part of the ear canal, approximately at the location of the osteochondral junction.
Etiologically significant pathogens
Almost always it is Pseudomonas aeruginosa.
Treatment
In patients with diabetes, treatment requires tight diabetic control, regular ear cleaning, topical antibiotic drops, and long-term, high-dose oral ciprofloxacin, usually for many months. Surgical clearance of residual masses is warranted in rare cases, and supplemental hyperbaric oxygen therapy is also used in severe cases.
Leakage of cerebrospinal fluid
CSF leakage from the ears occurs due to congenital or acquired pathology of the temporal bone in combination with a perforated eardrum. Congenital causes often occur with defects in the development of the labyrinth or roof of the middle ear (tegman tympani), and are often combined with meningoencephalocele in the mastoid process. Acquired pathology is associated with a fracture of the temporal bone or surgery on the mastoid process or labyrinth.
Symptoms
History of head injury or surgery. Clear fluid coming from the ear and/or nose. Other symptoms may occur as a result of the underlying condition causing the CSF leak, such as dizziness, hearing loss, and tinnitus.
Signs
Quite often, pulsating fluid leaking from the perforated eardrum is visible. Other symptoms of a basal skull fracture or previous surgery may be evident.
Treatment
Collecting fluid and asking for beta-2-transferrin can confirm the presence of CSF. Often only one drop of liquid is needed for analysis. An absorbent stick inserted into the ear can help collect fluid.
It is appropriate to advise a patient with a recent traumatic CSF leak to move the bed to a semi-sitting position and avoid sneezing or coughing. Up to 80% of traumatic CSF leaks resolve spontaneously within seven days, and almost all CSF leaks resolve within six months. CSF leakage from the ear of traumatic origin ends spontaneously more often than traumatic CSF rhinorrhea.
CSF leakage from the ear requires a visit to your local ENT department. X-ray examination is often required and surgery is rarely required.
Polyps/granulation tissue
Patients will often complain of chronic ear discharge that may contain blood. Bloody discharge is often associated with a polyp in the ear. The etiology of polyps can be determined by the location of the polyp in the ear canal. Granulation tissue is often present after mastoid surgery or as a result of chronic infection. Polyps can be a manifestation of either a chronic middle ear infection or a chronic outer ear infection. Polyps that develop in the posterior superior quadrant or pars flaccida are often associated with cholesteatoma. Polyps that develop at the junction of the bony and cartilaginous portions of the ear canal may be due to malignant otitis externa.
Ear carcinoma
This condition is rare. Patients usually complain of pain and bloody discharge from the ear, which continues despite local and/or systemic antibiotic treatment. Patients may eventually develop symptoms of intracranial extension of the process, such as meningitis and/or cranial nerve palsy. Patients may have a history of chronic ear discharge due to chronic suppurative otitis media. Such patients should be referred for ENT consultation if urgently indicated.
Complications of suppurative otitis media
The spread of infection beyond the middle ear can be a consequence of both acute and chronic suppurative otitis media. The incidence of such complications has decreased significantly with the introduction of antibiotics. Traditionally, the presence of cholesteatoma has been considered a more dangerous condition compared with mucinous suppurative otitis media without cholesteatoma. Browning studied 26 consecutive cases of brain abscess that were thought to develop in the setting of chronic suppurative otitis media. Cholesteatoma was present in 12 (46%) of these patients, mucosal disease without cholesteatoma was present in 10 (38%), and mastectomy was performed in 4 (15%) patients. Browning concluded that the absence of cholesteatoma, or previous mastectomy, should no longer be considered a safe situation.
Although rare, complications of chronic suppurative otitis media can be life-threatening. Complications can be categorized as intracranial or extracranial. A list of potential complications is provided in the table below. It is important to be aware of the presence of these conditions, as prompt management of these complications is critical.
| Intracranial | Lateral venous sinus thrombosis; Meningitis; Epidural, subdural, intracerebral abscess. Hydrocephalus associated with otitis media |
| Extracranial | Otitis externa; Erosion of the auditory bone; Middle ear commissures; Sclerosis of the tympanic membrane; Squamous cell carcinoma of the middle ear; Facial nerve paresis; Labyrinthitis; Petrositis (inflammation of the pyramid of the temporal bone); Labyrinthine fistula |
Treatment often includes high doses of intravenous antibiotics, treatment of the underlying disease, and involvement of a neurosurgeon in cases where intracranial abscesses develop.
Ear drops for perforated eardrum
The use of ototoxic drops in the presence of a perforated eardrum is a matter of debate due to evidence of sensorineural hearing loss as a result of these drugs. Data on such associations are rare and the significance of these reports is often in question. Of course, the risks of sensorineural hearing loss or major complications of otitis media, which underlies the disease, and the fact that these medications are highly effective in treating the underlying infection are also of great importance. Limiting the course of treatment with potentially ototoxic ear drops, and making sure they are not used on healthy (dry) ears, can reduce any potential risks from prescribing ototoxic medications. Clinical guidelines for the prescribing of ototoxic drops have been developed in the UK and the reader is provided with the following information. The important point is that these drops should only be prescribed for a short period of time in the presence of a specific infection. Patients should be warned about the potential side effects when using this type of medication, and patients are advised to stop using these types of medications if they increase symptoms of significant dizziness.
What other treatments are available?
For all clinical conditions, there are a number of approved and unapproved treatments for ear discharge. Hyperbaric oxygen therapy is rarely recommended for severe malignant otitis externa, although there is insufficient evidence to support its effectiveness in a systematic review of clinical cases. Much non-medical literature concerns earwax production as a cause of ear discharge. But the production of earwax is a normal physiological process, and the only problem is when the earwax blocks the ear canal. There are a number of topical treatments and devices that can be sold over the counter to remove earwax, although most of these treatments have not been rigorously scientifically tested. Ear candling has been suggested to remove earwax using smoke or a burning candle. This practice is condemned in the medical literature due to the fact that it is ineffective for removing earwax and is also potentially dangerous for the wax to melt into the ear canal, however, the popularity of this method seems to continue.
See also, Antibiotic therapy for acute otitis media in children
Diagnostics
The symptoms that accompany the discharge can tell a lot. However, a doctor cannot make a correct diagnosis based only on the patient’s complaints. In this case, you will need to undergo a full examination, which includes:
- Taking a smear for bacteriological examination.
- Audiometry.
- MRI;
- CT.
Often people ignore the doctor’s request to take all tests and undergo a full examination, since they believe that there is no need for this. Allegedly, a diagnosis can be made simply by looking at the ear and studying the characteristics of the fluid flowing from it. But that's not true. There are many pathologies and most of them have similar symptoms. And in order to choose the right therapy that will really help eliminate the problem, you need to be examined completely!
Don’t ignore your body’s signals: if clear fluid is flowing from your ear!
Ear discharge is a liquid type object that tends to flow out of the hearing aid, that is, from the ears.
Such an object can have a fairly varied color (cloudy, yellow, brown, red or transparent).
In this case, the discharge can be either quite abundant or sometimes random. This manifestation can be seen in the morning on the pillow after sleep.
Discharge
Quite often, many people confuse the concept of fluid discharge from the ears. Sometimes people think that the wax that accumulates in the ear is this fluid.
Yes, sulfur sometimes occurs in liquid form, but sulfur is not a pathological formation .
In this case we are talking about purulent discharge. They are exclusively inflammatory diseases that usually affect the outer and middle ear. These include:
- external types of otitis
- fungal inflammation of the ear, which is called otomycosis
- various boils that have broken open. This is an inflammation of the sebaceous glands of the auditory passages, which ultimately forms a confined cavity. This cavity is filled with pus
- an acute type of otitis media that damages the eardrum itself in the ear
- chronic otitis in the acute stage
- various injuries of the ear and eardrum in particular
- various tumors of the middle or outer ear
Causes of white and watery, odorless
- Various ruptures in the eardrum, which is accompanied by otitis media (this situation leads to the accumulation of fluid in the middle ear, but without any signs of inflammation)
- Inflammation of the ear skin due to allergic reactions . This applies to the skin that lines the outer ear
- Leakage of cerebrospinal fluid, which is fluid from the spinal cord, due to a head injury . In this case we are talking about damage to the skull up to its fracture
It is very important to determine the color of the leaking liquid at the very beginning; based on this information, the cause and type will become clear. It can be transparent, purulent, or brown, white, or more watery.
Character
- The browner color resembles sulfur, which is what most people confuse with sulfur or vice versa;
- Experts call the white color cheesy;
- There is also black color of fluid from the ear;
- If the fluid is purulent in origin, then it is yellow, green or gray;
- And finally the bloody color.
The very process by which discharge from the ear occurs indicates an inflammatory process in the human body. Professionals call this origin otorrhea .
It is by determining the type of liquid, that is, its color, consistency, and other physical parameters, that one can determine the cause of its occurrence, as well as the type of disease that affects the discharge.
If the liquid is presented in a transparent color, then this is an exacerbation of a certain allergy, and this indicates the beginning of the development of otitis media . The development of infection in the body makes itself felt in the form of a yellow or white tint of fluid that comes from the ear.
In this case, purulent inflammation of the spinal cord is possible. If the discharge is bloody in consistency and color, then this indicates so-called polyps , which are contained in the auditory opening.
Regardless of the color of the liquid, you should consult a doctor, and self-medication is not recommended.
The clear liquid itself is not a disease . The reason for this discharge is another disease or an inflammatory process in the body. When treating, it is necessary to act exclusively on the cause, that is, on the disease itself. Also, clear liquid may be a symptom of one or another allergic reaction.
There are situations when you started using certain drops for your ears, and then liquid began to flow, this indicates an allergy. In this case, the drops should be put aside and consult a doctor.
Also, the first stages of otitis media make themselves felt precisely due to discharge from the ears. There are also cases when a simple runny nose with prolonged manifestation can lead to discharge from the ears. If there are certain particles of blood in the discharge, then so-called polyps may have formed in the ear.
The reason for the clear type is a disease.
The most common disease in this case is exudative otitis media . This is a disease that is the accumulation of so-called serous effusion in the ear cavity. It is the appearance of such fluid that indicates to us that perforation of the ear membrane has occurred. This process occurs due to the effect of pressure on the membrane itself.
What needs to be done in such a situation?
There are situations when this liquid neutralizes itself, but this is very rare.
But it also happens when the fluid accumulates and is not able to come out, in which case treatment is required.
Moreover, treatment in this case must be carried out extremely quickly , since this exudate can destroy the integrity of the membrane and it will rupture, which will lead to hearing problems.
Exudate can be eliminated through so-called pneumomassage or by blowing with a certain tube . You cannot blow it yourself; this process occurs under the supervision of doctors and by the doctors themselves. As a result, the functions of the ear will be completely restored, and the fluid itself will be successfully removed.
Conclusion
If fluid accumulates in the ear canal and comes out of it, then you need to seek help from specialists . In this case, it is absolutely not advisable to ignore the problem.
If you ignore the problem, this leads to the so-called addition of a bacterial or fungal infection to this process.
If we allow this stage of the disease to progress, the color of the liquid will completely change.
Source: https://dr-lor.com/uho/simptomy/vydelenija-uho/prozrachnaya-zhidkost.html
Treatment
The appearance of discharge has different etiologies. Thus, their therapy is also different in nature. Thus, with the development of purulent otitis, antibacterial solutions are used, which are instilled into the ears several times a day, and with otomycosis, agents with an antifungal effect are used.
If there are boils in the ear canals, they are opened, and then a course of antibacterial therapy is prescribed. In case of allergic otitis, drugs that have an antihistamine effect are used. If the discharge causes a traumatic brain injury, you should definitely consult a neurosurgeon, since only he can help in this situation.
There is no single treatment regimen for discharge. Therapeutic measures are selected individually and, above all, they depend on the cause of the problem, the patient’s age and his general health. Therefore, only a doctor can choose the right treatment. But under no circumstances should you self-medicate. This can negatively affect your health.
Causes of otorrhea
In order to determine the treatment method, it is necessary to establish why fluid is secreted in the ear. The factors that provoke this symptom are different:
- Complications of external and otitis media. This is a disease characterized by an inflammatory process in the cavity of the outer or middle ear, respectively. The main symptom is severe ear pain. With proper treatment, discharge from the ears is not typical for otitis, but if measures are not taken in time, pus accumulates in the cavity behind the eardrum. He puts pressure on the membrane until it breaks and releases the accumulation of pus out. Since the pressure on the membrane stops, you can hear from the patient that “his ear is leaking, but it doesn’t hurt.” A decrease in pain does not negate the need for specialist consultation and treatment. Purulent otitis is dangerous because of meningitis, encephalitis and mastoiditis.
- Inflammation of the middle ear, which is of an allergic nature. This condition is easily treated with antihistamines. The fact that the ear does not hurt makes some patients put off going to the doctor. This is a big mistake, since, firstly, only a specialist can make an accurate diagnosis, and secondly, he will select the optimal treatment method that will relieve symptoms in the shortest possible time.
- Mastoiditis, or inflammation of the mastoid process of the temporal bone. The disease is not a pleasant one, but it can be prevented by timely and adequate treatment of otitis media. With mastoiditis, the discharge can be purulent in nature (in this case we speak of purulent mastoiditis) or yellowish, resulting from swelling.
- Fracture of the skull bones. This injury may damage the dura mater. Then cerebrospinal fluid is released from the nose and ears - colorless and odorless. Of course, medical attention is required immediately to avoid death.
- Cyst-like cholesteatoma is diagnosed in the case of epithelial growth in the middle ear. The neoplasm cells secrete a yellowish secretion with an unpleasant odor that flows from the ear. An urgent visit to an otolaryngologist will reduce the risk of irreparable consequences, which include death.
- Furunculosis, or the accumulation of foci of inflammation of the sebaceous gland, is a relatively harmless cause of pus discharge from the ear. When pathogenic bacteria enter the ear canal, inflammation may occur in the form of a pimple, in the center of which there is a sac with purulent contents. It is this that flows out of the ear at the stage of tissue necrosis. At any stage of development of furunculosis, the pathology requires treatment.
- Otomycosis. In other words, this is ear fungus, which occurs as a result of the proliferation of the fungus against the background of weakened body resistance (often the result of excessive effort when cleaning the ears from wax). The ear does not hurt, but it itches and is very sensitive. The disease may be accompanied by scanty brown or black discharge from the ear.
Doctors' recommendations
Discharge from the ears is accompanied by:
- hearing loss;
- pain;
- dizziness;
- the appearance of ear noise;
- black spots are found in the discharge;
- lymph nodes enlarge.
If your ear suddenly starts to leak, it's otitis media. What should not be done during otitis media?
- Compresses and heating pads are contraindicated before visiting a doctor.
- Do not reduce the course of prescribed medications on your own.
- It is strictly forbidden to use anti-inflammatory or alcohol-based drugs without a doctor’s prescription.
The lack of appropriate treatment for otitis in children can be quite dangerous and cause a decrease in auditory activity. The ears hurt, as a result the child will be restless. It is worth calling your local pediatrician.
Fluid like water may come out of your ears. At the same time, there is a very strong feeling of pain in the ears.
The causes of discharge can be a variety of pathologies of other anatomically related organs.
The lack of appropriate treatment for otitis in children can be quite dangerous and cause a decrease in auditory activity. The ears hurt, as a result the child will be restless. It is worth calling your local pediatrician.
Fluid like water may come out of your ears. At the same time, there is a very strong feeling of pain in the ears.
The causes of discharge can be a variety of pathologies of other anatomically related organs.
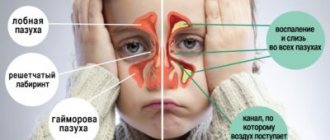
The ears are interconnected with the throat, nose, nasopharynx and oral cavity. For example, if the teeth are affected, this will affect the ears, so the pain will occur at the same time. In addition to the leaking fluid, the head hurts severely, then you need to urgently call a doctor.
general characteristics
There are a number of factors that can provoke the described symptom. These factors can be both natural and pathological.
Natural causes
It is also necessary to know that when fluid flows from the ear, it can be caused by a number of natural causes that are not direct signs of some developing pathology, but indirectly indicate its likelihood. In such cases, these manifestations do not require independent treatment as such, however, there is a need to eliminate the actual reason why fluid flows from the ear. Natural causes include the following:
- hypothermia, in which the glands activate, aimed at protecting the ear canals from the cold;
- overheating of the body;
- getting water or other liquid into your ears;
- sudden changes in atmospheric pressure;
- neglect of personal hygiene, as a result of which wax plugs form in the ears, getting rid of which, the body intensively secretes fluid from the ears;
- overzealous ear hygiene, which damages the tissues lining the ear canals, resulting in inflammation;
- excessive physical activity, during which too strong jumps in blood pressure occur in the body;
- severe stress;
- hormonal disorders.
In any case, even if, after eliminating the provoking factor, the symptoms disappear, the first thing to do if fluid is flowing from the ear is to consult a specialist, since this symptom, even in the absence of any discomfort, can be alarming a sign indicating the presence of a serious pathology.
Causes of a pathological nature
The discharge of fluid from the ear almost always signals some kind of disorder. How serious these disorders are, and how to treat the ears if they are leaking, can only be decided by a qualified specialist, for this pathology - an otolaryngologist.
This situation is especially dangerous if, along with the discharge of fluid from the ear, the patient is bothered by such manifestations as:
- itching in the ears and in the area around them;
- discomfort and pain;
- swelling and redness of the outer ear;
- temperature increase;
- weakness, decreased performance;
- nausea, tinnitus, dizziness.
The symptoms described above indicate that an active inflammatory process is occurring in the body, during which the body’s defenses are activated, and various types of discharge appear as a reaction to disturbances. The causes of this phenomenon may be various imbalances in the microflora of the inner ear, the presence of pathogens - bacteria, and also, possibly, a foreign object located in the ear canal, for example, an insect that has got there, or a small toy if the patient is a child.
The accumulated fluid in the ear is a special secret that helps the body get rid of the cause that provoked the inflammation, purely mechanically - by washing it out of the ear canal.
There are a number of specific pathologies in which fluid forms in the ears. These diseases include the following:
- otomycosis, that is, fungal infection of the ear canal;
- purulent otitis, characterized by the presence of infectious or mechanically provoked inflammation of the epithelium lining the surface of the inner ear;
- bullous otitis media, resulting from the development of a viral infection;
- furunculosis, that is, inflammation of the hair follicles and adjacent tissues;
- mechanical damage to the skull;
- mastoiditis, which is a complication that occurs with otitis media;
- polyps in the ears, which are benign growths of cells in the mucous membrane lining the inner ear;
- cholesteatoma, a neoplasm similar to a tumor, affecting the mucous and connective tissue;
- myringitis, in which the eardrum becomes inflamed;
- seborrheic dermatitis, which is an inflammation of the sebaceous glands.
Depending on a particular pathology, the ear leaks, accompanied by some accompanying manifestations. Each of the diseases listed above has its own symptoms. In particular, the color and nature of ear discharge can vary significantly.