This is an insidious disease: its first signs can be confused with a simple malaise.
The best way to Early TB detection to catch an incipient disease is to undergo fluorography annually or do skin tests (for example, Mantoux). But if for some reason you missed the test, there is still an option to recognize tuberculosis by its early symptoms. This will help you survive.
According to the World Health Organization, tuberculosis is one of the 10 most common causes of death in the modern world.
But let's start with something more important.
Why do you need to do fluorography or skin tests, even if everything is fine with you?
There is a high probability that you are already infected with mycobacterium tuberculosis - Koch bacillus. You just don't know about it. And you won't find out unless you take a diagnostic test.
The fact is that doctors divide tuberculosis into two forms Tuberculosis.
Not everyone who gets infected gets sick. Many people's immune systems are strong enough to suppress the activity of tuberculosis bacteria. As a result, the Koch bacillus is present in the body, but there is no tuberculosis. However, he can prove himself.
Approximately two billion people worldwide have latent tuberculosis.
The probability that the latent form will develop into an active one, according to WHO Tuberculosis, is 5–15%. The risk increases if you have a condition that weakens your immune system. These could be pregnancy, liver and kidney diseases, diabetes, malnutrition (addiction to strict diets), smoking, oncology or HIV infection.
Since a decrease in immunity sometimes occurs quite quickly, it is worth finding out in advance whether you are infected with a latent form of tuberculosis. With information about this, your doctor will be able to offer you preventative treatment. This will prevent Tuberculosis (TB) tuberculosis from developing into an active form.
Occurs when the immune system cannot control the growth of bacteria. Having this form of the disease, a person not only risks his own health, but also actively infects others.
https://youtu.be/https://www.youtube.com/watch?v=QbUrkCHTeRU
_
Methods for treating tuberculosis without coughing:
Medication methods
If detected in time, the disease can be treated. The course duration is usually 6 months. Treatment may take longer depending on the complexity of the case. As a rule, the latent or asymptomatic form of the disease, when the patient does not have a cough or fever, results in severe complications due to the fact that tuberculosis is not detected immediately. By the time an accurate diagnosis is established, pathogenic bacteria have affected internal organs, and treatment becomes much more complicated and delayed.
To treat tuberculosis, including the form without cough, antibacterial drugs are used to combat Koch bacilli. Medications are also used that can eliminate the complications that arise. Doctors do not recommend interrupting treatment until complete recovery, since there is a high probability of developing drug resistance and progression of the disease with renewed vigor. Long-term exposure to medications can cause toxic effects on the patient's body. Phthisiatricians recommend the use of hepatoprotectors. The most effective drugs are Isoniazid and Rifampicin. They are well tolerated by patients weakened by the disease and are not as toxic as other drugs.
If drug treatment does not have the desired effect, doctors may resort to surgery. After the disease is defeated, the patient needs to maintain his immune system and monitor his health. The recovery period after suffering from tuberculosis involves visiting sanatorium-resort establishments and adhering to a certain regime and diet.
What to do if you notice symptoms of tuberculosis
This has been said many times, but we will repeat: immediately make an appointment with a therapist. The specialist will listen to your story about your symptoms, look at your medical history and offer tests that will confirm or refute the preliminary diagnosis.
Perhaps in your case the cause of the illness is not tuberculosis at all. And even if he does, today this disease is treatable (of course, when the process has not gone too far). It is only important to identify it early and begin to treat it. Don't hesitate.
Got a cold? - those around him are interested in a coughing person. But not only ARVI, but also dozens of other diseases can manifest themselves in this way
When a cough appears, all the characteristics of this symptom are studied:
Duration. A cough that lasts more than 3 weeks is chronic. Until this time, it is considered acute.
Duration. On this basis, it is divided into episodic, short-term, paroxysmal and constant.
Timbre. There are dry, wet, barking, spasmodic coughs, etc.
Character. A non-productive cough does not bring relief, but a productive cough (with sputum), on the contrary, helps the body get rid of harmful substances.
The situation in which the symptom appeared. For example, a cough may occur during a certain season or a specific time of day. It can begin after an infection and as a result of taking medications, eating, changing body position, and also in response to external stimuli.
The patient has professional contact with harmful substances, allergies and specific complaints indicating concomitant diseases.
Possible causes of acute cough:
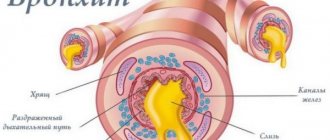
Acute and obstructive bronchitis
Details. Most often occurs with acute respiratory viral infections (influenza, measles, whooping cough, etc.). A sharp increase in temperature (up to 38.5–39°), low chest cough with copious sputum production, general malaise. The cough usually gets worse at night when lying on your back. With obstructive bronchitis, a painful paroxysmal cough is accompanied by difficulty breathing, wheezing (spastic cough).
What to do.
Treatment is mainly symptomatic: fever reduction, inhalations, expectorants. For bacterial bronchitis, antibiotics may be needed.
Acute pharyngitis, laryngitis, laryngotracheitis
Details. With laryngitis, the cough is painful, dry, and the voice is hoarse. Children may develop a dangerous narrowing of the larynx (croup), accompanied by difficulty wheezing and a barking cough. With pharyngitis - severe soreness, tingling or pain in the throat, which forces the patient to cough to get rid of the feeling of a lump stuck in the throat.
What to do.
See an ENT doctor and do a laryngoscopy. Treatment usually requires antibiotics. In case of false croup, immediately call an ambulance - in most cases it is difficult to eliminate laryngeal swelling on your own.
ARVI, flu
Details. Dry cough turning into wet cough. Sputum can be clear (a sign of a viral infection) or purulent (which indicates a bacterial infection). Other signs: increased body temperature, runny nose, weakness, malaise.
What to do.
Use antiviral treatment. For wet coughs, medications that thin the mucus and make it easier to clear help.
Whooping cough
Details. Develops gradually. A spastic dry cough appears, the intensity of which constantly increases (up to the appearance of vomiting).
What to do.
The diagnosis is made based on the determination of high levels of antitoxic antibodies in the blood. Antibiotics, sputum-thinning medications, and fresh air help.
Pneumonia and pleurisy
Details. At the beginning of the disease there is a dry cough, then a wet paroxysmal cough. Lobar pneumonia is characterized by a sudden onset with fever, chills, pain in the chest and ribs when breathing, and rust-colored sputum. With pneumonia caused by Friedlander's bacillus, the discharge is brick-colored or the color of currant jelly. With an infection caused by staphylococcus, the sputum is salmon-colored; Streptococcus produces purulent sputum, mycoplasma bacteria produces thick bloody discharge.
With pleurisy, the cough is dry, with a predominant stabbing pain in the chest, aggravated by coughing and deep breathing.
What to do.
The main diagnostic method is x-ray of the lungs, the main method of treatment is antibacterial therapy.
Pulmonary tuberculosis
Details. A moderate to severe wet cough may be accompanied by hemoptysis. Prolonged fever, night sweats, swollen lymph nodes. Sputum can be either scanty and mucous or profuse and purulent.
What to do.
Contact a phthisiatrician and get an x-ray of the lungs, and also conduct repeated (at least 3 times) microbiological examination of sputum for tuberculosis pathogens (the most informative method is PCR).
Possible causes of chronic cough:
Bronchial asthma
Details. Cough, shortness of breath and wheezing often occur at night, as well as after exercise, exposure to cold or after contact with an allergen. During an attack, viscous sputum with clots is released.
What to do.
Contact an allergist and pulmonologist. Carry out skin tests (for allergens), spirometry (respiratory function test), peak flowmetry (determining peak expiratory flow (PEF). A decrease in PEF by more than 20% of normal is a sign of asthma.
Idiopathic cough
Details. It is recorded in 20% of patients when the cause of cough, even after an active examination, cannot be determined. Typically, middle-aged women suffer, who develop a long-lasting dry cough during menopause, often after suffering from acute respiratory viral infection.
What to do.
Alas, all that remains is to limit ourselves to the use of antitussive drugs.
Sinusitis, sinusitis, allergic and vasomotor rhinitis
Details. Cough occurs due to the fact that copiously secreted mucus from the nose flows down the back wall of the pharynx into the trachea. Frequent coughing (especially at night), as well as symptoms such as nasal congestion, runny nose, and difficulty in nasal breathing are typical.
What to do.
Contact an ENT doctor and have your nose treated. The diagnosis is made based on examination.
Subscribe to our Telegram. Get only the most important things!
The World Health Organization has named Russia among the countries where drug-resistant forms of tuberculosis are spreading faster than in other countries. This means that the disease, which usually recedes after a standard course of antibiotic therapy (in the middle of the last century, tuberculosis was considered defeated), becomes difficult to treat.
Tuberculosis is accompanied by an increase in body temperature (37.5 - 38.5 degrees). Moreover, both day and night, the temperature remains stable, staying at the same level: it does not decrease in the morning, and does not rise in the evening, as happens with a common cold. This causes excessive sweating and a cough, which can be either dry or wet.
It is impossible to determine without tests that the cause of a cough is not tuberculosis. Therefore, doctors warn: if the cough does not disappear within two weeks (especially if the patient is undergoing treatment), additional examinations are needed. We are talking not only about a fluorographic image of the lungs, but also about sputum analysis. It is needed to find out whether there is mycobacterium (the causative agent of tuberculosis) in the body. If the result is positive, the patient is sent for treatment to a department where patients with open tuberculosis are treated. This form of the disease is dangerous for others, that is, such people can infect others. And you can get infected from a person who does not yet know his diagnosis anywhere.
For example, if you work in the same office with such a patient and often come into contact with him. Or even in transport. Then the risk group primarily includes children, the elderly, cancer patients and those who have chronic diseases. The state of the immune system is of decisive importance, because bacteria can enter the body, but the disease will not develop. The person becomes a carrier. And the impetus for the development of tuberculosis can be hypothermia, stress, chronic diseases, and bad habits. Therefore, salvation is only in a healthy lifestyle and annual preventive examinations.
A person may not feel that he has such a serious illness. The problem is that tuberculosis does not always manifest itself symptomatically, or the symptoms are not pronounced. It all depends on the functioning of the immune system. If the immune system is strong, then tuberculosis may not manifest itself at all. That is, a person maintains an active lifestyle, works, but only feels a certain weakness. But usually in such cases everything is attributed to overwork. A fairly typical situation is when, during a regular examination, doctors note changes in a patient’s lungs, although the person has no complaints about his health. Tuberculosis may not appear for a long time - from several months or even up to a year. The danger comes from a patient who coughs (then a pathogenic bacterium is released). It happens that it all starts with a mild cough, and the body temperature may not even rise. Then the patient reassures himself that it is a mild cold, just drink some syrups and everything will go away. But several weeks pass and the cough does not go away.
The spread of the disease is also facilitated by the fact that tuberculosis patients are forced to live next to healthy people, in cramped apartments, use shared kitchens and toilets, but the sick should be isolated until they stop shedding the infection. A special topic is our colonies and isolation wards, which, it’s no secret, have turned into a breeding ground for Koch’s bacilli.
It is not without reason that experts have placed Russia among the alarming list of countries where drug-resistant forms of tuberculosis have appeared. After all, in addition to other troubles, we have a common medical and social problem: many people are not treated correctly. Even with high-quality antibiotics. Treatment of tuberculosis is incompatible with alcohol and cigarettes, since this negates all therapy, and many patients ignore this attitude. And then these people become a source of infection for others. The antibiotic-resistant tuberculosis bacillus, when it enters the body of a child or adult with a weakened immune system, develops very rapidly. Accordingly, doctors will have to look for special compositions of chemotherapy drugs, rather than the usual antibiotics, and this complicates treatment.
The problem is also exacerbated by the low level of hygiene in families where people with open tuberculosis live. If such patients are not isolated, then the infectious diseases hospital regime must be in effect in the room at all times (disinfection, wet cleaning, separate utensils). Otherwise, the sick infect the healthy.
All iLive content is reviewed by medical experts to ensure it is as accurate and factual as possible.
We have strict sourcing guidelines and only link to reputable sites, academic research institutions and, where possible, proven medical studies. Please note that the numbers in parentheses ([1], [2], etc.) are clickable links to such studies.
If you believe that any of our content is inaccurate, out of date, or otherwise questionable, please select it and press Ctrl + Enter.
There are two forms of nasal tuberculosis: primary (lupus and tuberculoma) and secondary (ulcerative caseous tuberculosis of the nose and bone tuberculosis of the nose). The cause is mycobacteria.
Tuberculous lupus of the nose belongs to the class of extrapulmonary tuberculosis with damage to the skin and subcutaneous tissue of various locations.
Tuberculous lupus of the nose affects women more often (65%). Lesions of the nose account for 63%, cheeks - 58%, ears and periocular surfaces -14%, in 13% of cases the red border of the lips is affected.
Tuberculosis, cold or pneumonia?
In our article today:
Tuberculosis, colds or pneumonia?
The World Health Organization names Russia among the countries with drug-resistant forms of tuberculosis
are spreading faster than in other countries. This means that the disease, which usually recedes after a standard course of antibiotic therapy (in the middle of the last century, tuberculosis was considered defeated), becomes difficult to treat.
Tuberculosis is accompanied by an increase in body temperature (37.5 - 38.5 degrees). Moreover, both day and night, the temperature remains stable, staying at the same level: it does not decrease in the morning, and does not rise in the evening, as happens with a common cold. This causes excessive sweating and a cough, which can be either dry or wet.
It is impossible to determine without tests that the cause of a cough is not tuberculosis. Therefore, doctors warn: if the cough does not disappear within two weeks (especially if the patient is undergoing treatment), additional examinations are needed. We are talking not only about a fluorographic image of the lungs, but also about sputum analysis.
It is needed to find out whether there is mycobacterium ( the causative agent of tuberculosis)
). If the result is positive, the patient is sent for treatment to a department where patients with open tuberculosis are treated. This form of the disease is dangerous for others, that is, such people can infect others.
And you can get infected from a person who does not yet know his diagnosis anywhere...
For example, if you work in the same office with such a patient and often come into contact with him. Or even in transport. Then the risk group primarily includes children, the elderly, cancer patients and those who have chronic diseases.
The state of the immune system is of decisive importance, because bacteria can enter the body, but the disease will not develop. The person becomes a carrier. And the impetus for the development of tuberculosis
may become hypothermia, stress, chronic diseases, bad habits.
Therefore, salvation is only in a healthy lifestyle and annual preventive examinations.
A person may not feel that he has such a serious illness. The problem is that tuberculosis does not always manifest itself symptomatically, or the symptoms are not pronounced. It all depends on the functioning of the immune system. If the immune system is strong, then tuberculosis may not manifest itself at all. That is, a person maintains an active lifestyle, works, but only feels a certain weakness. But usually in such cases everything is attributed to overwork. A fairly typical situation is when, during a regular examination, doctors note changes in a patient’s lungs, although the person has no complaints about his health...
Tuberculosis
may not appear for a long time - from several months or even up to a year. The danger comes from a patient who coughs (then a pathogenic bacterium is released).
It happens that it all starts with a mild cough, and the body temperature may not even rise. Then the patient reassures himself that it is a mild cold, just drink some syrups and everything will go away.
But several weeks pass and the cough does not go away.
Therefore, let us be attentive to our health. And, very important, you should undergo regular examinations. But tuberculosis feels confident in our country and there are many problems with this. – untreated tuberculosis
in the usual form.
This is what gives the bacteria time, so to speak, to come to its senses and strengthen itself. And this happens for various reasons; often there is simply not enough medicine in medical institutions. But it also happens that in the presence of antibiotics, patients at their own discretion stop therapy prematurely.
Standard course – 4 – 6 months. The “unfinished” Koch stick is gaining strength, and the next time an exacerbation occurs, you will need not just a large dose of medicine, but completely different drugs (more expensive).
If a standard course costs up to 5,000 rubles, for the treatment of multidrug-resistant tuberculosis - 5,000 - 50,000 dollars.
The spread of the disease is also facilitated by the fact that tuberculosis patients are forced to live next to healthy people, in cramped apartments, use shared kitchens and toilets, but the sick should be isolated until they stop shedding the infection. A special topic is our colonies and isolation wards, which, it’s no secret, have become a breeding ground for Koch’s bacilli. Resistant forms are characterized by systemic damage to the respiratory system (broncho-obstructive syndrome), severe damage to the lungs, parallel heart problems (signs of dilated cavities), the appearance of high body temperature, and at the same time weight loss, the release of bacteria (this can be seen from the results of laboratory analysis ). In general, tuberculosis in such forms is more severe. A person “melts” and “burns” before our eyes.
It is not without reason that experts have placed Russia among the alarming list of countries where drug-resistant forms of tuberculosis have appeared. After all, in addition to other troubles, we have a common medical and social problem: many people are not treated correctly. Even with high-quality antibiotics.
Treatment of tuberculosis is incompatible with alcohol and cigarettes, since this negates all therapy, and many patients ignore this attitude. And then these people become a source of infection for others. Antibiotic-resistant tuberculosis bacillus
, when entering the body of a child or adult with a weakened immune system, it develops very rapidly.
Accordingly, doctors will have to look for special compositions of chemotherapy drugs, rather than the usual antibiotics, and this complicates treatment.
The problem is also exacerbated by the low level of hygiene in families where tuberculosis patients
in an open form. If such patients are not isolated, then the infectious diseases hospital regime must be in effect in the room at all times (disinfection, wet cleaning, separate utensils). Otherwise, the sick infect the healthy.
Source: https://medblock.ru/medicina_i_zdorovje/535-tuberkulez-prostuda-ili-vospalenie-legkih.html
Pathogenesis and pathological anatomy
Tuberculous lupus of the nose occurs as a result of the spread of MBT by hematogenous and lymphogenous routes from endogenous foci in other organs. Sometimes, usually in childhood, exogenous infection occurs, caused by massive infection of damaged skin. There are localized and disseminated forms of skin tuberculosis. Tuberculous lupus of the nose is a localized form and affects the skin of the nose, its mucous membrane, spreading to the oral mucosa. The primary element is a tubercle (2-3 mm in diameter) - a lupoma of a round shape, with clear boundaries, soft-elastic consistency, brownish-pink color, painless on palpation. There are flat and early infiltrative forms of tuberculous lupus of the nose.
The flat form is an infiltrate formed by the fusion of the lupus, located in the dermis and almost not protruding above the skin level. The infiltrate has clear scalloped edges surrounded by a border of hyperemia. Its spread occurs due to the formation of new tubercles along the periphery. The surface of the infiltrate may be covered with silvery-white scales, warty growths, erosions and ulcers, or have other features.
The infiltrative form of tuberculous lupus of the nose is characterized by damage to the soft tissues of the cartilaginous part of the nose and nasolabial region, resulting in the formation of an infiltrate with unclear boundaries and peeling on the surface in the dermis and subcutaneous tissue. Healing of the infiltrate occurs with the formation of a deep disfiguring scar. With the long-term existence of a lupus lesion or scar, its malignization is possible: a dense, painful pinkish-bluish infiltrate appears with necrosis in the center, often covered with a black dense crust (lupus-carcinoma).
Clinical course and symptoms of nasal tuberculosis
The clinical course of tuberculous lupus of the nose is long, lasting for many years, interrupted by remissions, sometimes spontaneous recovery, but most often accompanied by spread to the mucous membrane of the neighboring respiratory and alimentary tract, lymphoid apparatus, auditory tube, up to the middle ear. The disease is accompanied by regional lymphadenitis.
A special clinical form of tuberculous lupus of the nose is bone tuberculosis of the sinus-nasal system. This form of tuberculous lupus of the nose is characterized by the occurrence of specific periostitis and osteitis, followed by so-called cold abscesses that form fistulas, caseous-necrotic tissue decay or the formation of pseudotumoral tuberculoma, most often localized in the area of the upper alveolar process. Patients complain of pain in the area of the base of the nasal pyramid, canine fossa and superciliary ridges, in accordance with which of the air systems is affected - respectively, the cells of the ethmoid labyrinth, the maxillary or frontal sinus.
In the initial period, paleness of the skin over the affected area is observed, and sometimes submandibular lymphadenitis. Non-ulcerated tuberculous nodules and infiltrates are detected on the nasal mucosa. During endoscopy of the maxillary or frontal sinus using a universal endoscope, the mucous membrane appears spotted with alternating areas of hyperemia and caseous yellowish deposits. The presence of these changes in the mucous membrane indicates the transition of the inflammatory process to a mature stage.
The mature stage of the rhinosinus form of lupus is characterized by caseous-necrotic decay of the soft and bone tissues of the affected area, the formation of fistulas and the release of purulent and caseous masses from them. Most often the maxillary sinus is affected in the area of the alveolar process. The osteoperiostitis that occurs here has an extensive growth and is accompanied by bleeding and neuralgia of the second branch of the trigeminal nerve. With frontal localization of lupus, osteitis is localized in the area of the frontonasal suture or in the area of the cribriform plate. When localized in the ethmoid bone, the process takes on a pseudotumorous form with the formation of caseous fistulas in the area of the internal angle of the orbit or in the cribriform plate, which often leads to a serious complication - tuberculous meningitis. Damage to the sphenoid sinus is characterized by the same changes as lesions to the ethmoid bone; in this case, the optic nerves, cavernous sinus and pituitary gland are at risk of damage. Lesions of the paranasal sinuses are accompanied by purulent-caseous discharge from the nose.
[1], [2], [3], [4], [5], [6], [7], [8], [9], [10], [11]
Today, tuberculosis is one of the most dangerous and severe infectious diseases.
Mortality from tuberculosis is about 30% of the total number of diagnosed cases. In 92% of cases, the tuberculosis process affects the lungs.
Effective treatment of tuberculosis in adults is possible only with timely detection and adequate therapy. It is necessary to know the first symptoms of the disease, what measures should be taken, and seek medical help in time.
Modern medicine is well acquainted with the signs of tuberculosis and has an extensive knowledge base regarding the diagnosis and treatment of this disease.
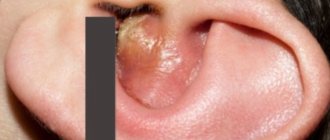
Nasal tuberculosis: symptoms, treatment and prevention
Nasal tuberculosis is a rare disease that affects patients with tuberculosis of the lungs, lymph nodes or bones. Occurs most often at a young age. Tuberculosis bacteria enter the nasal mucosa through the lymphatic or circulatory system. Infection of the nasal mucosa occurs mainly sputogenically (through sputum) if there is an open form of tuberculosis.
In rare cases, infection through lymph or blood (lymphogenous or hematogenous) is possible.
Clinical picture
There are three forms of upper respiratory tract tuberculosis:
- Ulcer.
- Infiltrate.
- Chondroperichondritis.
Infiltrate is an accumulation of tuberculous tubercles in the subepithelial tissue, around which there is connective tissue that is not subject to sclerosis, but has a tendency to subsequently grow. The lesion spreads diffusely, including to the glands.
As reactivity decreases, the local process worsens, the subepithelial tubercles disintegrate, and ulcers appear. Further, the process goes deep into the nasal mucosa, especially in the presence of a secondary infection.
Symptoms
At the initial stage of the disease, symptoms are mild. As the infiltrates grow, it becomes more difficult for the patient to breathe.
When the infiltrates disintegrate and ulcers appear, the appearance of specific discharges is noted - purulent or mucopurulent, in rare cases mixed with blood.
When the discharge dries, it causes difficulty in nasal breathing and itching in the nose. By removing dried masses from the nose on your own, the patient risks damaging the tuberculosis ulcer and causing bleeding.
Symptoms also include mild pain in the nose and severe nasal congestion.
Diagnostics
It is not difficult to diagnose the disease if there are other tuberculosis foci.
To distinguish tuberculosis of the upper respiratory tract from syphilis, it is necessary to keep in mind that tuberculosis affects exclusively the cartilage tissue of the nose, and syphilis, in addition to cartilage, affects the bone.
In addition, syphilitic diseases are characterized by a pungent odor resulting from bone necrosis, as well as severe pain in the nasal area. No similar symptoms were noted with tuberculosis.
Pain can only occur with tuberculous periostitis of the nasal bones, but this disease is extremely rare.
The symptoms of nasal tuberculosis and nasal cavity cancer sometimes coincide so much that a correct diagnosis can be made only on the basis of histological examination.
In case of tuberculoma, a biopsy is performed to exclude the diagnosis of sarcoma.
Diagnosing the disease is more difficult if the patient has no manifestations of tuberculosis damage to other organs. If such symptoms are present, there is more reason to talk about this particular diagnosis.
Treatment
Treatment should be long-term and comprehensive and begin immediately after diagnosis. As with any form of tuberculosis, etiotropic therapy is used for nasal tuberculosis. Taking into account the prevalence of the process, general and local therapy is carried out.
The main drugs for the treatment of this disease are:
- Phtivazid.
- Para sodium aminosalicylate (PAS sodium).
- Streptomycin.
In addition to the above-mentioned drugs, their analogues can also be used in the treatment of the disease.
Acids (for example, lactic, trichloroacetic, parachlorophenol) are widely used to cauterize tuberculosis infiltrates. Experts note the highest efficiency when using parachlorophenol. This substance was first used for the treatment of tuberculosis by otorhinolaryngologist, academician N.P. Simanovsky.
An ointment based on pyrogallic acid (10–20%) and potassium iodide for internal use are also prescribed for a period of 4 to 8 weeks.
Individual tuberculosis lesions can be removed by surgery (excision of the affected part of the nasal septum) or by electrocoagulation.
A significant effect was noted when the nasal mucosa was irradiated with quartz through a tube. Facial defects resulting from nasal tuberculosis can be corrected by resorting to plastic surgery.
This should be done only after the underlying disease has been completely cured.
Hygiene, climate and diet play an important role in the treatment of nasal tuberculosis.
Prevention
Preventive measures against upper respiratory tract tuberculosis include:
- Sanitation of the upper respiratory tract.
- Quitting bad habits (smoking and excessive alcohol consumption).
- Possible change of professional activity (under unfavorable working conditions).
- Spa treatment.
Risk factors
It is widely believed that tuberculosis is a disease that affects asocial elements and people with difficult living conditions. This is not true; every adult has a risk of becoming infected.
A third of the world's population is infected with tuberculosis. However, the role of the social factor in the spread of tuberculosis is very high.
Categories of the population that are more susceptible to infection:
- people with severe infectious diseases, especially chronic stages;
- HIV-infected and AIDS patients;
- people with diseases of the endocrine system, especially diabetes;
- patients taking certain drugs that reduce the body’s defenses, patients on dialysis and after organ transplantation;
- people suffering from drug addiction;
- people in prison;
- people without a fixed place of residence or leading an antisocial lifestyle.
You can also identify age categories with a high probability of contracting tuberculosis: these are children under 10 years of age and elderly people over 60 years of age.
This is due to the fact that the immune system in childhood and old age does not work as efficiently.
The risk of contracting tuberculosis increases if there is constant contact with an infected person. This category includes medical personnel working with tuberculosis patients. With one-time contact, the likelihood of infection is lower than with regular interaction.
You need to know that mycobacteria remain viable in an open environment for quite a long time and are resistant to most disinfectants.
Koch's wand, once in the body, may not manifest itself in any way. In order for pulmonary tuberculosis to move from a latent form to an active one, the body must experience stress. The progression of the disease can be triggered by infection, a sharp decrease in immunity due to poor nutrition, exposure to unsanitary conditions, and abuse of alcohol and drugs.
Diagnosis and possible complications of tuberculosis
It is very important to notice the first signs of illness. It is important to remember that while in the incubation period, the first signs of tuberculosis in adults can be mistaken for a common cold. First of all, a number of studies are carried out to diagnose the disease:
- general analysis of the patient's blood and urine;
- fluorographic or x-ray examination;
- Mantoux test;
- sputum analysis;
- bronchoscopy (instrumental examination of the lungs);
- PCR diagnostics, which includes a detailed blood test of the patient;
- in some cases, puncture or biopsy of the affected areas is possible.
After a set of tests, the form and stage of the disease is determined, a course of antibiotic therapy is prescribed, and in some cases surgery is performed.
During the treatment period, the patient must be in a special tuberculosis dispensary under the supervision of TB doctors. The duration of treatment is quite long, from several months to several years.
Important! In the early stages of the disease, it is difficult to make an accurate diagnosis, since the symptoms are very similar to ARVI or bronchitis. It is for this reason that it is important to seek advice from a doctor at the first sign of any cold, rather than self-medicate.
The first manifestations of tuberculosis
The appearance of the first symptoms of pulmonary tuberculosis depends on the individual physiological and pathogenetic data of a particular patient.
The severity of symptoms depends on how much time has passed since infection, as well as on the state of the body’s defenses, the presence of concomitant diseases, working conditions, climatic conditions, and the influence of external factors.
After a person is infected with Koch's bacillus, a long time may pass before the first signs of the disease appear. If the immune system copes with its functions, then its cells easily repel the attack of the aggressor.
A person may not even suspect that he is sick for a long time, even if the disease occurs in an open form. This is due to the fact that the disease in the early stages does not manifest itself with severe symptoms. And if there are any ailments, a person most often takes them for signs of other diseases.
Such camouflage is one of the main dangers of tuberculosis.
The main symptom of tuberculosis is the separation of sputum interspersed with blood. But in the early period it manifests itself only if the infection is massive and the disease progresses rapidly.
At first, pulmonary tuberculosis produces symptoms characteristic of many infectious diseases. These include: general malaise, low-grade temperatures, profuse night sweats, dry non-productive cough, headaches, a complex of asthenic symptoms, and lack of appetite.
Depending on the general state of health, symptoms such as rapid heartbeat, hypotension, lymphadenitis, and liver hyperplasia may appear. In most cases, a neurological syndrome is formed.
Its manifestations include:
- irritability;
- nervousness;
- dizziness;
- decreased performance;
- fast fatiguability;
- sleep disturbances, apathy.
The first signs of pulmonary tuberculosis that appear can be mistaken for symptoms of infectious diseases of the upper respiratory tract. Some ignore the appearance of neurological manifestations, attributing them to fatigue, constant busyness and other realities of life.
Clinical picture
There are three forms of upper respiratory tract tuberculosis:
- Ulcer.
- Infiltrate.
- Chondroperichondritis.
Infiltrate is an accumulation of tuberculous tubercles in the subepithelial tissue, around which there is connective tissue that is not subject to sclerosis, but has a tendency to subsequently grow. The lesion spreads diffusely, including to the glands.
As reactivity decreases, the local process worsens, the subepithelial tubercles disintegrate, and ulcers appear. Further, the process goes deep into the nasal mucosa, especially in the presence of a secondary infection.
Detection of tuberculosis in the early stages
A combination of specific signs allows identifying pulmonary tuberculosis in the early stages. It is necessary to undergo regular medical examinations, scheduled diagnostic examinations, and fluorography.
Tuberculosis manifests itself as a complex of various symptoms. An experienced specialist, having compared and analyzed the anamnesis data, can suspect the presence of this severe pathology in the patient and prescribe tests and studies.
What signs indicate the presence of pulmonary tuberculosis?
Causes
To know where tuberculosis comes from, it is necessary to study in more detail information about its causative agent. This microbacterium is resistant to external influences, high-temperature influences, and remains viable for a long time at low temperatures.
Infection with Koch's bacillus is what causes pulmonary tuberculosis. By the way, it is not listed as a highly contagious infectious agent. Despite the fact that a carrier of a virus with an open form of the disease emits bacteria into the environment, the likelihood of getting sick after contact with the pathogen and its entry into the body in a healthy person is extremely low.
A person with tuberculosis does not need to be treated under observation in a hospital if the disease is inactive. He is not limited in movement and social activity. But with continuous household contact, in families where there is a person sick with tuberculosis, it is recommended to pay attention not only to his well-being, but also to maintaining hygiene, measures to increase the immunity of other family members and constant checks of the body’s reaction to the Mantoux test to determine the likely infection at the most early stages.
Among the conditions that reduce specific immunity and contribute to the development of the disease, upon contact with an infected representative, the following reasons why tuberculosis appears are distinguished:
- Tobacco smoking. This is a condition for the development of diseases of the bronchopulmonary system, which reduce local immunity.
- Frequent consumption of alcoholic beverages.
- All types of drug addiction.
- Predisposition to diseases of the respiratory system due to the presence of structural pathologies, a history of intense illnesses, and the presence of chronic inflammatory processes in the respiratory organs.
- Chronic diseases and sources of inflammation in other organs and tissues.
- Diabetes mellitus, endocrine diseases.
- Unbalanced diet, lack of vitamins and nutrients.
- Neurotic pathologies, depressive states, low stress tolerance.
- Pregnancy period.
- Unfavorable social and living environment.
If we find out what causes tuberculosis in children, then the main reason in this case is contact with an infected person. After all, as you know, this disease is transmitted by airborne droplets.
Cough with pulmonary tuberculosis
Tuberculosis of the lungs is characterized by chest symptoms, the main of which is cough.
If any cough does not go away within two or three weeks, you should immediately consult a pulmonologist and undergo an examination. As a rule, in the early stages, the patient’s cough is dry, with a small amount of sputum produced.
The most severe coughing attacks torment the patient in the morning, after assuming an upright position. This is due to the fact that during a period of prolonged stay in a horizontal position, the sensitivity of the mucous membrane decreases, a significant amount of sputum accumulates in the upper respiratory tract, and when changing position, it causes the urge to cough.
As the disease progresses, exudation begins, cavities form, and the cough intensifies and can appear at any time of the day. A characteristic symptom is incessant coughing attacks.
The patient choke and suffocate, but until the airways are cleared at least a little, the cough does not stop. If the disease becomes a closed focus, the cough may disappear altogether.
Diagnostics
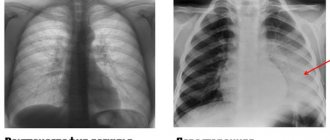
The pulmonary form of tuberculosis is diagnosed mainly during fluorographic examination.
The study reveals fresh and old lesions in the form of lesions, infiltration or cavities. After identifying the disease, a blood test is done.
In the presence of fresh foci, neutrophilic leukocytosis is detected with a shift of the formula to the left. If the disease occurs in a severe form, lymphocytosis with pathological granularity of neutrophils is detected in the blood. In the acute period, ESR levels increase.
Sputum culture is another important test to determine the presence of Koch's bacillus.
If an x-ray shows the presence of a cavity, then mycobacteria are almost always detected in the culture. It is extremely rare that Koch's bacillus is sown if an x-ray shows the presence of a cavity. Typically, 3 sputum cultures are performed.
When conducting a mass examination, a test for tuberculosis is carried out. The Mantoux test shows the presence of a skin reaction after the administration of tuberculin.
If there is no infiltrate, the sample is negative; if the infiltrate is 2–4 mm in size, the sample is doubtful. If the size of the infiltrate exceeds 5 mm, the test is considered positive. In addition to illness, a positive reaction may be caused by recent vaccination. What kind of doctor treats the disease - a phthisiatrician.
https://youtu.be/https://www.youtube.com/watch?v=EVn5lutxvEQ
_
Temperature
One of the main signs of tuberculosis is a slightly but constantly elevated temperature.
Usually during the day the body temperature is within the normal range, increases in the evening, and is accompanied by feverish symptoms and chills.
The use of antipyretics either does not have an effect or briefly reduces the temperature, causing profuse sweating, headache and general weakness. If this symptom continues for more than two or three weeks, it means that the infectious process is progressing and you should immediately consult a doctor.
Signs by type of disease
Tuberculosis takes extrapulmonary forms and affects the internal organs of a person. It is classified depending on its location. There are the following types of tuberculosis with the following symptoms:
- Bones and joints. Such localization of the disease in question almost never causes difficulties in diagnosis. The discs between the vertebrae become deformed, causing compression and the formation of a hump. The knee and hip joints are also affected, leading to arthritis and bone pathologies. As a result, a person cannot climb stairs or walk several meters without assistance.
- Genitourinary system. A complex of symptoms of urological disorders appears: bloody impurities are observed in the urine, pain is felt in the lumbar region and ovaries. For females, the manifestation of this pathology is dangerous due to the inability to conceive, and for males - the development of varicocele and a space-occupying formation in the scrotum.
- Skin. Characteristic is the development of dense nodular formations under the skin, which increase in size as the disease progresses. When the nodules are opened, discharge in the form of a white curd mass is observed.
- Nervous system. Central nervous system lesions are diagnosed in young children and HIV patients. Symptoms include migraines, mental disorders, epilepsy, tinnitus, poor coordination, eye pathologies, short-term fainting and sometimes seizures.
- Gastrointestinal tract organs. Accompanied by general signs of tuberculosis with disturbances in the digestive process, discomfort in the intestines and bloody stools.
- Kidney. Symptoms manifest as nephritis, but may be completely asymptomatic.
- Brain. It occurs more often in people with obvious signs of immunodeficiency and endocrine diseases. It differs from other diseases in the gradual development of symptoms. The primary symptoms are headaches and insomnia. A week later, patients report pain in the back of the head and forehead, and neurological disorders. After two weeks, the headaches become intense and are accompanied by vomiting.
- Miliary tuberculosis. Characterized by the spread of mycobacteria throughout the body's bloodstream. Tuberculous tubercles form in various organs. It has the character of a typhoid-like disease.
Important information: What are the symptoms of pulmonary tuberculosis in adults and how to quickly cure
Chest pain
The tuberculosis process in the lungs is often accompanied by pain in the chest area, in the hypochondrium area, which intensifies with movement. In cases where the disease affects, in addition to the lungs, the pleural cavity, the pain is more pronounced.
Spirometry reveals slow breathing on the affected side, which is the reason for conducting studies to detect tuberculosis.
Symptoms of tuberculosis without cough
Clinical symptoms of the disease are a painful cough and high fever. If they are absent, you should pay attention to the following manifestations of the disease:
- Painful blush on the face or excessive pallor.
- Shortness of breath, which occurs not only during active activities, but also at rest.
- Suffocation. In the final stages of tuberculosis, the lung volume of the infected person decreases, and functional tissue is replaced by scar tissue. Against the background of these processes, a person loses the ability to breathe normally.
- Pain in the chest and back. The pain intensifies when trying to breathe.
- Increased volume of regional lymph nodes.
- Anemia. Signs of anemia are drowsiness, pallor, dry skin, brittle nails and hair, hair loss, apathy, and weakness.
- Poor appetite.
- Sudden unexplained weight loss.
- Chronic fatigue.
- Heavy sweating, especially at night.
- Gurgling and wheezing when breathing.
Lymphadenitis
One of the first symptoms of tuberculosis is enlarged lymph nodes. Most often, the lymph nodes under the arms, behind the ears and on the neck become enlarged. This phenomenon is painless.
Laboratory tests during this period do not show significant changes in the blood count, but the disease progresses.
Tuberculosis is extremely difficult to detect in its early stages. The clinical picture of symptoms in the initial period of the disease is erased. There are either no symptoms at all, or they are similar to the manifestations of other infectious diseases.
Laboratory tests at an early stage can show the absence of pathogens in the test material. Under these conditions, diagnosis is significantly difficult. However, science does not stand still, and today doctors will be able to understand the pathogenesis of the disease even with minimal input data.
Therefore, you should not postpone a visit to a therapist, phthisiatrician or pulmonologist if at least a few symptoms of an unhealthy condition appear.
Symptoms
In the early stages of its occurrence, the disease may not have any pronounced symptoms. During this period, its manifestations include only increased weakness, sweating (more often it bothers the patient at night), weight loss, easy fatigue, apathy, and pallor. Some people may also experience a low-grade fever that cannot be caused by other factors. Often in such people tuberculosis is detected during a blood test or an X-ray of the lungs. In some cases, the disease cannot be identified at this stage.
Later, as the disease develops, the patient may develop specific symptoms. These include:
- Cough. In the initial stages of the disease, it can be dry and prolonged, and then becomes productive, accompanied by the discharge of sputum. This cough can bother the patient both during the day and at night. It should be noted that in the later stages of the disease, cough may be accompanied by hemoptysis.
- Labored breathing. In some cases, it may be accompanied by severe chest pain. It should be noted that the breathing of a patient with tuberculosis will be difficult both during physical activity and at rest (especially in the later stages of the disease).
- Elevated temperature. In this case, it indicates the course of the inflammatory process in the body.
- Runny nose. This symptom does not always accompany tuberculosis, but can occur with serious damage to the respiratory system.
In the later stages of the disease, the patient may also experience disturbances in the gastrointestinal tract and other body systems.
They are associated with the penetration of bacteria into these organs or systems. The appearance of such pathologies indicates complications of the disease.