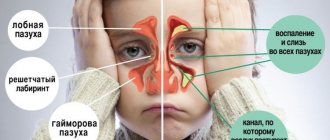
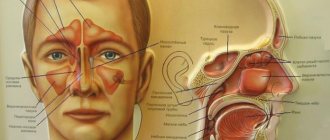
Anatomical structure of the paranasal sinuses
There are 4 paranasal sinuses in the human skull, named according to the bones in which they are located.
Frontal sinuses
The frontal sinuses are paired cavities located in the thickness of the frontal bone, behind the brow arches. Each of them communicates with the middle nasal passage through the frontonasal duct.
The frontal sinuses rarely have a symmetrical appearance; the septum between the left and right sinuses most often deviates to one side or the other. Average sizes:
- Height – 28 mm.
- Width – 24 mm.
- Depth – 20 mm.
The frontal sinus is lined internally with mucous membrane, communicating with the supraorbital nerve and receiving blood supply from the supraorbital and anterior ethmoidal arteries.
At birth, the infant has no frontal sinuses. They form as the child grows, reaching their normal size after puberty.
Lattice Maze
This is a group of small cells located on the side of each ethmoid bone. The ethmoid labyrinth is located in the skull between the upper part of the nasal cavity and the orbit.
All cells of the lattice labyrinth are divided into three groups:
- Posterior group - the lumen of the cells connects with the upper nasal passage, and sometimes with the sphenoid sinus.
- Middle - has an outlet into the middle nasal meatus.
- Anterior - also connects to the middle nasal meatus.
The ethmoidal labyrinth communicates with the anterior and posterior ethmoidal nerves, and receives blood supply from the ethmoidal and lacrimal arteries.
Sphenoid sinus
Each of the two sphenoid sinuses is located in the body of the bone of the same name. They can have different sizes and shapes, rarely being symmetrical. Each sphenoid sinus opens into the corresponding superior nasal meatus.
Approximate dimensions of the sphenoid sinus:
- Height – 2.2 cm.
- Width – 2 cm.
- Depth – 2.2 cm.
The mucous membrane of the sphenoid sinus is connected to the posterior sphenoid and facial nerves.
Maxillary sinus
The maxillary (maxillary) sinuses are the largest of all paranasal sinuses, located in the maxillary bone. It has a pyramidal shape and is located slightly below the nasal cavity. The maxillary sinus exits through the semilunar foramen into the middle meatus, below the opening of the frontal sinus. This arrangement of drainage holes contributes to the spread of the infectious process from one sinus to another.
The mucous membrane of the maxillary sinus is connected to the maxillary and facial nerves.
Paranasal sinuses
In humans, there are four groups of paranasal sinuses, named according to their location:
· maxillary (maxillary) sinus (paired) - the largest of the paranasal sinuses, located in the upper jaw.
· frontal sinus (steam room) - located in the frontal bone.
· ethmoid labyrinth (paired) - formed by cells of the ethmoid bone.
· sphenoid (main) sinus (unpaired) - located in the body of the sphenoid (main) bone.
The paranasal sinuses begin to form in utero and complete their formation after puberty. The inside of the sinuses is lined with ciliated epithelium with mucus-producing goblet cells. Through the movement of epithelial cilia, mucus moves to the openings of the paranasal sinuses at a speed of 1 cm/min. The hole sizes are small; Thus, in the cells of the ethmoid labyrinth the diameter of the holes is 1-2 mm.
Messages from the nasal cavity:
- communicates with the nasopharynx through the choanae;
- with the eye socket through the nasolacrimal canal. It opens into the lower nasal meatus.
- with air sinuses of the skull bones:
· frontal sinus – opens into the middle meatus;
· maxillary sinus – opens into the middle nasal meatus;
· cells of the ethmoid bone - open into the upper and middle nasal passages;
The sphenoid sinus opens into the superior nasal passage. In pathology, the infection penetrates from the nasal cavity into the sinuses and sinus inflammation develops - sinusitis (sinusitis, sinusitis, etc.).
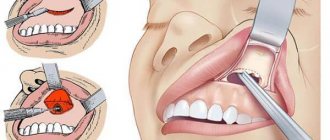
Puncture of the maxillary sinus is performed for both diagnostic and therapeutic purposes. Currently, puncture of the maxillary sinus for therapeutic purposes is the most effective way to evacuate purulent contents and administer an antiseptic for inflammation of the maxillary sinus (Fig. 2.26). However, this method is not popular in a number of foreign countries.
Before puncture, anemization of the mucous membrane in the area of the middle nasal passage is performed using vasoconstrictor drugs to cause contraction of the mucous membrane in the area of the natural anastomosis of the maxillary sinus and, therefore, facilitate the evacuation of fluid through the opening. The mucous membrane of the lower nasal passage is lubricated with topical anesthetics (2% dicaine solution, 5% cocaine solution, 10% lidocaine solution, 10% diphenhydramine solution, etc.). The optimal puncture site is at the top of the arch of the inferior meatus at a distance of approximately 1.5-2.0 cm posterior to the anterior end of the inferior turbinate. It is easier to make a puncture in this place, since there is a minimum thickness of the lateral bone wall of the nasal cavity. After installing the Kulikovsky needle
under the inferior turbinate, using the mobility of the cartilaginous part of the nose, the needle head is retracted in the medial direction so that the needle becomes as vertical as possible to the lateral wall of the nose and the sharp end is directed to the outer corner of the eye on the same side. The needle is grasped with the entire hand of the right hand so that its head rests in the palm, and the index finger is on the needle, fixing and guiding it. The puncture is made with moderate force with light rotational movements with a needle to a depth of approximately 10-15 mm. After making sure that the end of the needle is in the sinus, use a syringe to suck out the contents, and then wash the sinus with an antiseptic solution (furacilin, octenisept, chlorophyllipt, etc.). The liquid flows into the sinus through a needle, and pours out through the natural anastomosis of the sinus, entraining its contents. When washing, the patient's head is tilted forward and down so that the water pours out through the vestibule of the nose into the tray provided.
If you cannot pierce the wall, you should not force it, using great force. It is necessary to change the position of the needle, raising its end higher, or move slightly backward until a more pliable point is discovered.
In cases where the anastomosis becomes blocked as a result of a pathological process, a second needle is also inserted into the sinus through the lower nasal passage, and rinsing is performed through two needles. The presence of pathological contents in the washing fluid allows one to reliably recognize the nature of the disease.
18. Surgical anatomy of the major salivary glands. Topographic anatomy of the duct of the parotid salivary gland, submandibular gland. Clinical significance.
The salivary glands are a group of secretory organs of various sizes, structures and locations that produce saliva.
Three major salivary glands:
- Parotid gland (glandula parotidea)
Its inflammation is mumps (viral infection).
The largest salivary gland. Weight 20-30 grams.
Located below and in front of the auricle (on the lateral surface of the branch of the mandible and the posterior edge of the masticatory muscle).
The excretory duct of this gland opens in the vestibule of the mouth at the level of the second upper molar. The secretion of this gland is protein.
- Submandibular gland (glandula submandibularis)
Weight 13-16 grams. Located in the submandibular fossa, below the maxillohyoid muscle. Its excretory duct opens on the sublingual papilla. The secretion of the gland is mixed - protein - mucous.
- Sublingual gland (glandula sublingualis)
Weight 5 grams, located under the tongue, on the surface of the mylohyoid muscle. Its excretory duct opens on the papilla under the tongue along with the duct of the submandibular gland. The secretion of the gland is mixed - protein - mucous with a predominance of mucus.
Small salivary glands , 1–5 mm in size, are located throughout the oral cavity: labial, buccal, molar, palatine, lingual salivary glands (mostly palatine and labial).
1.Parotid gland, the largest of the salivary glands, serous type. It is located on the lateral side of the face in front and slightly below the auricle, also penetrating into the fossa retromandibularis. The gland has a lobular structure (Fig. 118), covered with fascia, fascia parotidea, which closes the gland into a capsule. The excretory duct of the gland, ductus parotideus, 5-6 cm long, extends from the anterior edge of the gland, runs along the surface of the m. masseter, passing through the fatty tissue of the cheek, pierces the m. buccinator and opens into the vestibule of the mouth with a small opening opposite the second large molar of the upper jaw. The course of the duct varies extremely. The duct is bifurcated. The parotid gland is a complex alveolar gland in its structure.
2. Submandibular gland, mixed in nature, complex alveolar-tubular in structure, second largest. The gland has a lobular structure. It is located in the fossa submandibularis, extending beyond the posterior edge of m. mylohyoidei. Along the posterior edge of this muscle, the process of the gland is wrapped onto the upper surface of the muscle; an excretory duct, ductus submandibularis, departs from it, which opens onto the sublingual gland.
Topography of the facial nerve on the face, area of innervation. Clinical manifestations of damage to the facial nerve and its main branches. Reconstructive operations for damage to the facial nerve.
Facial nerve, n. facialis
(Fig. 177), unites two nerves: the facial nerve itself,
p. facialis,
formed by motor nerve fibers - processes of the cells of the nucleus of the facial nerve, and the intermediate nerve,
p. intermedius,
containing sensitive taste and autonomic (parasympathetic) nerve fibers. Sensitive fibers end on the cells of the nucleus of the solitary tract, motor fibers begin from the motor nucleus, and autonomic fibers begin from the superior salivary nucleus. The nuclei of the facial nerve lie within the pons of the brain.
Arriving at the base of the brain at the posterior edge of the pons, lateral to the olive, the facial nerve, together with the intermediate and vestibulocochlear nerves, enters the internal auditory canal. In the thickness of the temporal bone, the facial nerve runs in the facial canal and exits the temporal bone through the stylomastoid foramen. In the place where there is a knee of the facial canal, the facial nerve forms a bend - the knee
and
the crank assembly.
The genu node belongs to the sensitive part of the facial (intermediate) nerve and is formed by the bodies of pseudounipolar neurons.
In the facial canal the following branches depart from the facial nerve:
1. Greater petrosal nerve, n. petrosus major,
formed by preganglionic parasympathetic fibers, which are processes of cells of the superior salivary nucleus.
This nerve originates from the facial nerve in the area of the knee and enters the anterior surface of the pyramid of the temporal bone through the cleft of the canal of the greater petrosal nerve. Having passed along the groove of the same name, and then through the foramen lacerum, the greater petrosal nerve enters the pterygoid canal and, together with the sympathetic nerve from the internal carotid plexus ,
is called the nerve
as part of the latter it approaches the pterygopalatine ganglion.
2. Drum string, chorda tympani,
formed by preganglionic parasympathetic fibers coming from the superior salivary nucleus and sensory (taste) fibers, which are peripheral processes of pseudounipolar cells of the genu ganglion. The fibers begin on the taste buds located in the mucous membrane of the anterior two-thirds of the tongue and the soft palate. The chorda tympani departs from the facial nerve before it exits the stylomastoid foramen, passes through the tympanic cavity without giving off branches there, and exits it through the tympanic-petrosal fissure. The chorda tympani then moves forward and downward and joins the lingual nerve.
3Stapes nerve, n. stapedius,
originates from the facial nerve and innervates the stapedius muscle.
After leaving the stylomastoid foramen, the facial nerve gives off motor branches to the posterior belly of the supracranial muscle, to the posterior auricular muscle - the posterior auricular nerve, p. auricularis posterior,
and to the posterior belly of the digastric muscle -
digastric branch, digdstricus,
to the stylohyoid muscle -
stylomastoid. sublingual branch, g. stylohyoideus.
Then the facial nerve enters the parotid salivary gland and in its thickness is divided into a number of branches that connect with each other and thus form the parotid plexus. This plexus consists only of motor fibers.
Damage to the facial nerve along its entire length causes peripheral paralysis of the facial muscles. In this regard, facial asymmetry arises, which is quite pronounced at rest and, especially when showing teeth (44, 45), when the corner of the mouth is not pulled back (m.risorius paralysis), and the “exclamation mark” phenomenon occurs. On the affected side, there is a smoothness of the folds of the skin of the forehead and nasolabial fold, the palpebral fissure is widened, it is not possible to close it while closing the eyes, since the eyelids do not close (paresis orbicularisoculi), while the eyeball turns upward (Bell's phenomenon), and through the uncovered a gap formed between the upper and lower eyelids, a strip of sclera (lagophthalmus) is visible; profuse lacrimation is possible from the widened palpebral fissure. It is impossible to wrinkle the forehead on the affected side, cause tension in the broad muscle of the neck, movements such as whistling, kissing, etc. become impossible. The patient experiences difficulty while talking and eating (food gets stuck between the cheek and teeth).
All surgical interventions for facial paralysis are divided into the following groups:
1. Restoration of facial nerve function (decompression, neurolysis, suturing of the damaged facial nerve and plastic with a free graft). 2. “Revival” of the function of facial muscles by operations on the sympathetic nervous system. 3. Reinnervation of facial muscles by suturing the facial nerve with other motor nerves (hypoglossal, accessory, phrenic). 4. Dynamic suspension of paralyzed parts of the face. 5. Static suspension of paralyzed parts of the face. 6. Corrective operations :
a) on the side of paralysis, b) on the healthy side - myotomy, neurotomy.
Functions of the paranasal sinuses
Scientists do not yet fully know what role the paranasal sinuses play in the human body.
At various times, theories have been proposed that the sinuses are involved in the resonance of the voice, are needed to warm the inhaled air, provide protection to sensitive structures (for example, tooth roots and eyes), promote facial growth, lighten the facial skull to maintain head position, secrete mucus for moistening the nasal cavity. However, all of them were refuted by further research.
The sinuses play an important role in the immune defense of the nasal cavity. Their mucous membrane produces nitric oxide, which has antiviral and bacteriostatic effects.
Types of inflammatory reactions
Treatment of any inflammatory reaction affecting the sinuses requires careful diagnosis of the disease. To do this, differential diagnosis is carried out according to three main criteria.
It will also be interesting: What does mucous discharge in women mean?
First of all, it is determined which cavity was damaged as a result of the inflammatory reaction:
- with pathology of the maxillary cavities, hamoritis develops;
- in case of pathology of the adnexal cavities, I diagnose ethmoiditis;
- if the frontal cavities are affected, then frontal sinusitis is diagnosed;
- with pathology of the sphenoid sinus, sphenoiditis is diagnosed.
After it is determined which sinuses are affected, the type of inflammation is determined. Inflammation of the sinuses can be:
- acute - symptoms usually appear abruptly, depend on the season and are observed for several weeks;
- chronic - symptoms are observed with regularity, there are periods of rapid development and periods of remission.
It is also important to establish what form of the inflammatory process. There are three in total:
- in the edematous-catarrhal form, the upper layers of the mucosa are affected;
- in the purulent form, deeper layers are affected;
- with a mixed form, different forms of inflammation are observed in different areas.
Methods for studying PPN
During an external examination, it is impossible to see the paranasal sinuses, so various instrumental studies are used to diagnose their diseases:
- X-ray of the sinuses . Normally, the sinuses are filled with air. That is, if in the conclusion a radiologist writes that the paranasal sinuses are pneumatized, this means that they do not contain liquid (blood, mucus, pus) and there are no benign or malignant tumors.
- A CT scan is a series of X-rays that are processed by a computer to produce a detailed image of an organ. Modern multislice computed tomography (MSCT) allows you to create three-dimensional images. MSCT of the paranasal sinuses is one of the most accurate methods for diagnosing their diseases.
- Magnetic resonance imaging is a diagnostic method that uses a magnetic field and radio frequency waves to visualize organs.
- Ultrasound examination (ultrasound) is a method that uses ultrasonic waves to obtain images of internal organs and tissues. Ultrasound of the paranasal sinuses is rarely used, although it makes it possible to diagnose some of their diseases, including acute and chronic sinusitis.
Features of the location of the sinuses in the child’s body
The location of the paranasal sinuses in children differs significantly from the anatomical structure in adults. So, at birth, the baby has only 2 sinuses - the ethmoid and maxillary. Moreover, both of them are represented by small diverticula of the nasal mucosa in the thickness of the bones. The maxillary sinus is 10 mm long and no more than 3 mm in height and width. Only by the 6th year of life do the sinuses acquire normal shapes, and at 12 years of age they descend to the location characteristic of adults. The rudiments of the ethmoid labyrinth in a newborn are located directly above the rudiments of the teeth. As the child grows, the teeth move to their natural place, and the sinus rises up and takes on the dimensions inherent in it. Major development of the ethmoid sinus begins between the ages of 3 and 5 years. It is then that the number of cells and their size increases significantly.
Both the internal and external nostrils are always made of bone as well as cartilage and, in addition, are constantly covered with mucous membranes.
Structure of the paranasal sinuses. The human forced sinuses are a complex structure of several nasal cavities. They lie behind the external nose and between the individual linings of several bones of the skull. They are classified as the respiratory tract as they are connected to the nose, throat, trachea and bronchi respectively. There is also a connection to the middle ear.
The main sinus (sphenoid), just like the frontal sinus, begins to form only in the fourth year of the baby’s life. By the age of 6, their dimensions can be no more than 8x12 mm. There are often cases when, instead of two frontal sinuses, only one develops or both are absent.
Diseases of the paranasal sinuses
The most common diseases of the paranasal sinuses:
- Acute or chronic sinusitis is an infectious or allergic inflammation of the paranasal sinuses.
- Polyps are the presence of a benign tumor in the sinus cavity.
- Cancer is a malignant tumor in the sinuses.
Paranasal sinuses are air-filled cavities located in the thickness of the bones of the facial skull. Their role in the body remains not fully understood. Anatomical features facilitate the penetration of infection from one sinus to another, since all paranasal sinuses communicate with the nasal cavity.
Author: Taras Nevelichuk, doctor, especially for Moylor.ru
Structure of the upper respiratory tract
The clinical anatomy of the nose and paranasal sinuses has a very complex structure. The nose itself serves as the beginning of the human respiratory system and continues with a cavity connecting the upper respiratory tract with the paranasal sinuses.
At the base of the external nose is a skeleton of osteochondral tissue covered with skin. All elements of the organ consist of cartilage and bones and skin. In turn, the base and dorsum of the nose are composed of 3 types of bone elements, arranged in pairs. The cartilage system is also represented by three types, arranged in pairs.
Ethmoidal cells form several small air cells between the eyes. At birth, they fill with fluid and continue to grow until they are shaped like small pyramids and separated by a thin septum. The full functions of the paranasal sinuses are still debated, but some tasks are suspected. They reduce the overall weight of a person's head, especially the front and facial bones.
They improve voice resonance. The paranasal sinuses can act as a kind of buffer in the facial bumps. The caves isolate the sensitive nerve pathways of the teeth or eyes from fluctuations in the temperature of the incoming air. They humidify and warm incoming air when air flow slows in these regions. The paranasal sinuses regulate the intranasal pressure balance.
The space called the nasal cavity is located behind the oral cavity and is divided into 2 halves by a cartilaginous septum. It has 2 pairs of holes: front and rear. The anterior ones are called nostrils, and the posterior ones are called choanae, descending into the nasopharynx.
The nasal cavity is surrounded by the so-called paranasal sinuses. In medicine, they are divided into 4 pairs and can be: frontal, sphenoid, maxillary and ethmoid sinuses.
In addition, they serve an important function in the immune system, being able to catch pathogens before they enter the respiratory tract. Apart from this assumption about the functioning of the paranasal sinuses, it is also possible that they do not serve any direct biological function. That is, they may also be a sparda of actual biological adaptations that occurred during evolutionary evolution.
Here you will find the cure
In most cases, it is caused by a viral infection and goes away within 10 days. Inflammation of the paranasal sinuses is defined as inflammation of the mucous membrane that covers the walls of the cavities. Inflammation is divided into several degrees. Acute sinusitis is usually caused by a viral infection.
In addition, these cavities are located in the near and far parts of the skull. The course of pathologies in them differs somewhat. This is explained by the fact that the anterior sinuses are connected to the nasal cavity by the middle, and the posterior sinuses by the upper nasal passage. At the same time, the incidence rate of the posterior sinuses is much lower than those located in front.
A detailed diagram allows you to see in which area of the skull the paranasal sinuses are located.
Although the viral pathogen lasts only 7-10 days, the bacterial infection is more persistent. Chronic sinusitis lasts for more than three months and can have many different causes, which should be diagnosed individually once symptoms appear. Depending on which parts of the paranasal sinuses are affected by inflammation, complaints arise in different parts of the facial bones. Pain and pressure usually worsen with changes in body position, such as when a person lies down. Viral infections are curable, and antibacterial use may be considered for bacterial infections.
Sinus inflammation: types and symptoms
Depending on which sinus the inflammatory process occurs in, there are:
- sphenoiditis - inflammation affects the sphenoid sinus,
- sinusitis - the maxillary cavities are affected,
- frontal sinusitis - frontal areas are involved,
- ethmoiditis - the process occurs in the cells of the ethmoid labyrinth.
Inflammation of the mucous membrane can affect one or more sinuses at once. This inflammatory process occurs in different forms:
- acute form with pronounced symptoms,
- recurrent – with less pronounced repetition of signs of acute inflammation,
- chronic.
The chronic form of the inflammatory process, which most often affects the maxillary sinuses and slightly less frequently the frontal sinuses, lasts about 2-3 months, even if therapeutic measures are used. Signs of a chronic process include:
- Nasal discharge of purulent, mucous, watery or mixed consistency.
- Difficulty breathing due to blockage of the nasal passages.
- Sore throat and reflex cough arising from swelling of mucous masses in the back of the throat.
- Headaches, noted mainly in the nose, forehead and eyes.
- Impaired olfactory function.
- The growth of polyps from the paranasal sinuses into the nasal passages.
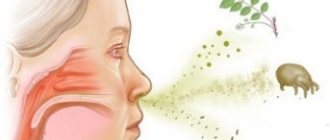
Unlike children, adults are more likely to experience a viral infection of the nasal mucosa, which spreads to the sinuses. Less commonly, blood diseases and dental conditions are the cause. The odontogenic factor is significant when the maxillary sinuses are affected. A viral infection, against the background of a “busy” immune system, can be accompanied by a bacterial factor, most often in the form of staphylococci, which can be activated.
Normally, microorganisms and microparticles, when inhaled, passing through the nasal cavity along with the air, enter the caves of the sinuses, where the ciliated epithelium captures them and neutralizes them to form mucus that is excreted. This mechanism can be disrupted by the curvature of various bone formations with anatomical deformation of the shells, as well as unfavorable factors affecting the protective properties of the epithelium: dry air, tobacco smoke, chemical burns, tissue atrophy and necrosis, depressed state of the immune system, etc. Edema can occur as well as a consequence of an allergic reaction.
Some of the most common general symptoms of sinus inflammation include:
- runny nose with thick greenish discharge and pus,
- headache, which intensifies with changes in pressure, when tilting the head, pressing on areas in the area of the nasal sinuses, as well as a feeling of fullness in these areas,
- condition of nasal congestion,
- increase in body temperature to 38C,
- morning and night cough.
Due to congestion, a person begins to breathe through his mouth and speaks in a nasal voice. In this case, there is often an unpleasant odor from the mouth.
With sinusitis, headaches associated with a pathological increase in intracranial pressure are one of the main symptoms. Pain in the forehead and sinuses can be pulsating or squeezing, which is typical primarily for the acute form. In addition to the above signs, the following is noted:
- decreased sense of smell (or loss of it),
- lacrimation and fear of light,
- sometimes – swelling of the upper eyelid or cheek.
In the chronic course of the disease, secretions flow down the wall of the pharynx, causing a night cough. In the mornings and evenings, there is a characteristic pain radiating to the area of the eye sockets. When pressing on the inner corner of the eyes, the pain spreads to the entire face.