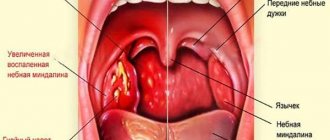
Sore throat during breastfeeding is an extremely dangerous phenomenon, fraught with a high risk of complications, because the disease is severe, and the process is complicated due to unwanted medications.
In the case of an inflammatory process in the tonsils, which are one of the natural barriers of the human body from the penetration of external infections, situations may arise that require the suspension of hepatitis B. The difficult decision on how to treat a sore throat during breastfeeding, how to get rid of it without medications, is made depending on the subclinical picture of the patient.
What is the danger of sore throat during lactation?
Tonsillitis or tonsillitis is a pathology known to mankind for thousands of years, the danger of which lies in its infectious origin. First of all, it poses a danger to the mother, because the presence in the body of a pathogenic agent (streptococcus, staphylococcus, virus or fungus) on the lymphatic pharyngeal ring or palatine tonsils indicates a weakened immune system.
For a breastfed infant, there is a high probability of transmission of a pathogenic agent that is absent during lactation. Only if the sore throat is mild (catarrhal), you can get by with folk remedies, home symptomatic treatment, started immediately, and the usual range of medications may not be required.
The range of treatment methods is limited; tonsillitis during breastfeeding often forces one to interrupt breastfeeding in order to prevent the development of complications in the mother and to protect the baby’s health from transmission of infection.
Antibiotics
It is not always possible to treat a sore throat during lactation without antibiotics. Sometimes purulent processes develop rapidly, and after 1-2 days a nursing woman notices symptoms of lacunar or follicular tonsillitis. In this case, only antibacterial agents can eliminate the infection and prevent severe complications of the disease. During breastfeeding, macrolides (sumamed, azithromycin, rovamycin), the latest generation penicillins (for example, amoxiclav, flemoxin), and some cephalosporins (for example, cephalexin) are allowed.
Tetracyclines and fluoroquinolones are strictly prohibited for a nursing mother, as these drugs can cause disruption of the baby’s hematopoietic system.
If a nursing mother has a high temperature, it can only be reduced with paracetamol-based products (but not acetylsalicylic acid). It is preferable to treat sore throat in short intensive courses (3-4 days), and at this time perform regular milk expression. According to WHO recommendations, taking the above antibiotics is not a reason even for a temporary pause in lactation, but during this period the child must receive medications against intestinal dysbiosis. Still, most breastfeeding experts believe that a break in feeding for several days will harm the baby much less than the existing effects of antibacterial therapy. To avoid having to treat a sore throat, during lactation you should dress warmly, avoid contact with patients, do not drink cold drinks and do everything to protect yourself and your baby from unnecessary risks!
Women who are pregnant and breastfeeding, unfortunately, get sick no less often than other women. And few people manage to do without medications. So, medications during pregnancy and breastfeeding: answers - Dr. Komarovsky.
We also recommend reading: sore throat in an infant.
First signs
The appearance of symptoms depends on the nature of the disease, the pathogenic agent, the appearance of which led to the development of the inflammatory process. Therapy for tonsillitis by the attending physician is symptomatic and prescribed depending on the data obtained during an external examination. Treatment of catarrhal tonsillitis lasts no more than 5 days, until the clinical symptoms disappear (film of exudate, low-grade fever, hyperemia of the tonsils. Pain in the throat disappears after inflammation.
Treatment of catarrhal tonsillitis during breastfeeding can be carried out without medications, but it depends on the cause that causes the sore throat, as well as how it manifests itself.
It is much more dangerous when a nursing mother develops a purulent sore throat. She gets:
- enlargement of adjacent lymph nodes, their compaction;
- a sharp rise in temperature;
- pain appears in the throat;
- other symptoms of acute inflammation (headache, increased fatigue, weakness, intoxication).
During this period, local immunity is very weakened, so the deterioration of the mother’s body quickly increases. The presence of the causative agent of the disease implies infection of the baby, whose resistance is completely dependent on immunoglobulins transmitted from the mother. Milk contains antibodies and can protect the baby from infection if there is no need to treat complications.
Prevention of sore throat in a nursing mother
To prevent tonsillitis, a nursing woman should be careful about her health. First of all, you need to avoid hypothermia, since most cases of sore throat occur in the autumn-spring period. It is also important to strengthen the immune system, for which you need to get enough vitamins from food or through various medications.
Even in ordinary people, tonsillitis can be quite severe and lead to the development of various complications. Therefore, treatment of sore throat during breastfeeding should be timely and include all the required drugs, both antimicrobial and restorative. If symptoms of tonsillitis appear, you should not self-medicate; it is better to consult a doctor. This is the only way to quickly and reliably get rid of inflammatory changes and prevent complications.
How to treat sore throat while breastfeeding
When breastfeeding, only the attending physician can decide how to treat a sore throat, after determining the nature of the pathological condition that caused the development of the process. Signs of inflammation and the severity of the condition are the main decisions in determining treatment tactics for a nursing mother.
The list of prescriptions and the drugs used are chosen after consultation with a doctor. The pathology can be of primary etiology due to hypothermia, or secondary, when the pathological process begins to develop against the background of influenza, acute respiratory infections or other viral infection.
Basic methods:
- rinses or inhalations, throat sprays allowed during pregnancy or lactation, lubricants, warm drinks;
- folk remedies prepared on the basis of medicinal plant and animal components;
- enhanced nutrition for a nursing mother to replenish the supply of vitamins, microelements, and restore immunity;
- restoratives to prevent the development of diseases against the background of an existing infection;
- drug treatment necessary for some forms of acute tonsil infection.
The addition of a secondary provoking factor requires the mandatory prescription of antiviral, antifungal or antibacterial drugs. When transmitted to a child, fungal tonsillitis (the treatment of which is associated with many difficulties at this age) can even pose a threat to his life.
Treatment with rinses, sprays and inhalations
How to treat sore throat while breastfeeding? The list of even local medications that are used for tonsillitis is more limited than in any other period of life. A young mother cannot use traditional remedies aimed at reducing pain, lowering temperature, and relieving inflammation. She is strictly contraindicated from taking any medications containing aspirin, ibuprofen or paracetamol. Homeopathic remedies with a similar range of actions are usually recommended; it is a good idea to gargle with furatsilin, use safe sprays that have no contraindications during lactation (Aqua Maris Spray, Ingalipt, Hexoral, Tantum Verde).
Hexoral is also available in the form of a solution used for inflammatory processes of the throat; you can prepare gargles from infusions of medicinal herbs that have anti-inflammatory and antiseptic effects.
Treatment with antibiotics for hepatitis B
Even if a threatening situation arises, only the attending doctor can authorize the use of antibacterial agents during lactation for treating a nursing mother. He will also turn to Amoxiclav, Sumamed and Ceftriaxone, not so much allowing them to be allowed for angina, but not prohibited, but will be able to take into account all the present contraindications. To achieve an effect, vitamins are often prescribed for a nursing mother.
Principles of treatment of disease during lactation
Depending on the suspected cause of inflammation, the doctor chooses antimicrobial or antiviral therapy. Treatment should be comprehensive and, in addition to drugs that act on the pathogen, it should be aimed at improving the patient’s condition and strengthening her immunity.
Traditional medicine alone should not be trusted, since it is not capable of completely destroying pathogenic microbes. This type of treatment is used to improve general condition. Therefore, before treating tonsillitis in a nursing woman, she should consult a doctor who will prescribe all the necessary medications depending on her condition.
Antibacterial agents
If the bacterial nature of the inflammation is suspected, antibiotics must be included in the treatment regimen. Treatment begins with the use of protected penicillins or cephalosporins of the first or second generation.
Any antibacterial medicine passes into breast milk in small quantities. Therefore, if it is necessary to use large doses of antibiotics, it is recommended to transfer the child to nutritional formulas for the period of treatment. A woman should pump at this time to prevent stagnation of milk and maintain the level of the hormone prolactin at the required level. Thanks to this, after recovery it will be possible to switch back to breastfeeding without any problems.
Treatment begins with taking Amoxiclav or Azithromycin tablets. If this approach is ineffective, they switch to intramuscular administration of drugs. The total duration of antimicrobial treatment for angina is 7-8 days.
Local treatment
Before treating a sore throat during breastfeeding with antibiotics, a specialist can also select local therapy. It is aimed at reducing the severity of inflammatory changes in the mucosa and the symptoms of the disease.
The most commonly used topical agents are:
- "Neo sore throat";
- "Bioparox";
- "Chlorophyllipt".
These are antiseptic drugs that help destroy bacteria on the surface of the tonsils. In addition, it is possible to use anti-inflammatory drugs and antipyretics. However, they should only be used when the temperature rises above 39 degrees.
Vitamins and other restoratives
In order for treatment for tonsillitis to be effective and quickly lead to recovery, you should use drugs that improve the overall resistance of the woman’s body. To do this, it is recommended to use products containing vitamins A, C and group B.
Folk remedies for sore throat
To reduce the severity of inflammation, herbal medicine is recommended. To do this, you can gargle with decoctions of various herbs: chamomile or calendula. In addition, gargling with saline solutions helps kill germs. It must be remembered that traditional methods are ineffective as independent treatment; they are used only in combination with other medications.
What you can and cannot eat and drink
In the acute period of the disease, when there are pronounced manifestations of inflammation of the tonsils, the patient is recommended to drink plenty of warm drinks. It allows you not only to replenish fluid loss, but also helps to remove the causative agent of the disease. To do this, it is better to use warm jelly, compotes, tea with lemon. Their temperature should be room temperature or slightly higher so as not to cause irritation to the inflamed mucous membrane.
The diet should be rich in protein and other nutrients. In this case, it is recommended to serve the dishes in grated or liquid form. You should also exclude hot, salty and spicy foods from your diet.
Child's reactions to mother's antibiotic treatment
Only medical supervision can prevent possible reactions of the baby to the mother’s antibiotic therapy. You should decide in time to stop using the pills. It is extremely undesirable to combine taking antibiotics and breastfeeding, but if it is necessary to maintain health during lactation, treatment is sometimes carried out with stronger drugs, stopping feeding the baby.
The use of antibacterial agents is also carried out with extreme caution. Some species that are still effective in the treatment of bacterial infections are strictly prohibited during lactation. Treatment of a nursing mother with such drugs can cause unwanted side effects in both mother and baby.
To prevent such conditions, it is necessary to take care of the woman’s health: it is necessary to protect her from contact with potential carriers of the infection. Vitamins for a nursing mother will be a good help for weakened immunity and help avoid illness.
The consequences of taking antibiotics are sometimes so negative that the patient is recommended hepatoprotectors and drugs to restore intestinal microflora, and this leads to the inability to continue breastfeeding after a sore throat.
Treatment
Most often, tonsillitis during lactation is primary and is caused by streptococcus. Such acute tonsillitis requires:
- Antibacterial local and general therapy.
- Application of vitamin complexes.
- Antihistamines.
- Detoxifiers.
- Antipyretics.
- And pro-(prebiotics) to compensate for the effect of antibiotic agents.
- A gentle diet.
- Drink plenty of fluids.
Sore throat during breastfeeding requires immediate specialist intervention and competent treatment. Experts rarely raise the issue of weaning a child due to the particular severity of the disease. But mom needs to follow several rules, in particular:
- Always wear a mask when feeding and interacting with your baby.
- You need to feed your baby in a well-ventilated area.
- The child should sleep separately from the sick mother.
With secondary and specific angina, a slightly different approach to treating angina in a nursing mother is required. The doctor focuses on treating the underlying disease. Antiviral drugs, antimycotics, and immunostimulating agents may be required.
General antibacterial therapy
Answering the question of how a sore throat is treated during breastfeeding, it should be said that for bacterial tonsillitis, general antibiotics are considered the first line of therapy. During the lactation period it is allowed to use in injection and tablet form:
- Cephalosporins (Cefazolin).
- Protected penicillins (Ampiox).
- Macrolides (Zitrolide, Azitrox, Sumamed, Azithromycin).
Whether it is possible to breastfeed with a sore throat and treatment with antibiotics is decided by the doctor. When prescribing the above groups of drugs, weaning the child from the breast is considered optional. If treatment with these drugs is ineffective and it is necessary to use those prohibited for breastfeeding, the child is removed from feeding.
The following groups of drugs are prohibited during breastfeeding: fluoroquinolones (Ofloxacin, Levofloxacin) and tretracyclines. If it is necessary to prescribe them, the mother of the child is weaned from breast milk during treatment. These drugs can affect the functionality of the baby’s hematopoietic organs and lead to serious disruption in the functioning of his internal organs.
The time required to treat this disease depends on the severity of the process and is about 7–10 days.
It is necessary to take into account the fact that in order to cure a mother’s sore throat, the doctor must prescribe her antibacterial agents; some of them will enter the baby’s digestive system. In order to prevent the death of the child’s natural intestinal microflora, he needs to be given means that help maintain it: pro-, pre-, symbiotics. Today, Simbiter, Maxilak, Bifinorm are popular.
Local antibiotics, antiseptics and sulfonamides
A doctor will tell you how to treat a sore throat for a nursing mother. But therapy for this disease is unlikely to be possible without local drugs. Such means include:
- Aerosols. Bioparox, Hexoral, Kameton, Ingalipt are popular both among doctors and patients.
- Tablets and lozenges. These include Faringosept, Septolete, Strepsils, Stop-Angin.
- Rinse solutions. Miramistin, Furacilin, Chlorhexidine are used as rinsing solutions.
The use of these means is not mutually exclusive. Aerosols can be used up to 3 times a day. The tablets are dissolved every 3 hours. You can gargle every 2 hours.
Nursing mothers are often interested in how this disease can be treated, since each of them wants to speed up the healing process. Lubricating the tonsils with Lugol's solution and gargling with Ectericide solution helps a lot with bacterial sore throat.
Symptomatic treatment
If a nursing mother’s sore throat is severe, with high fever, severe swelling of the tonsils, and headaches, doctors usually recommend a 5-day course:
- Antihistamines (Erius).
- NSAIDs (Paracetamol).
- Vitamin complexes.
Experts recommend lowering the high temperature, because the milk can “burn out” during acute inflammation. But such popular antipyretics and anti-inflammatory drugs as Aspirin or Nise are not recommended during the lactation period. At high temperatures, saline infusions may be prescribed to replenish circulating blood volume.
During breastfeeding, mothers are allowed vitamin complexes Elevit Pronatal, Vitrum Prenalal, Multi-tabs Perinatal. The doctor may recommend that some of his patients take it during the entire period of breastfeeding, and not just during the treatment of sore throat during lactation. Taking these complexes can help in the prevention of tonsillitis and in a speedy cure if the disease does overtake the woman.
Herbal medicine and traditional methods
At high temperatures, a woman loses a lot of fluid. You can compensate for its deficiency with the help of fruit drinks, juices, and dried fruit compotes. What other remedies does traditional medicine offer:
- You can drink chamomile decoction in limited quantities.
- It is good to gargle with a decoction of chamomile, sage, St. John's wort, and calamus root.
- You can dissolve 1 teaspoon of honey in the mouth if the baby does not have allergies. You can’t get carried away with honey, but it is a wonderful and tasty antiseptic.
You cannot be content with folk methods alone, since sore throat causes serious complications (from abscesses to rheumatism).
Alternative medicine should be used as an auxiliary therapy to the main one. These measures are very effective and breastfeeding is not a barrier to their use.
Diet and regimen
Treatment of sore throat during breastfeeding is not complete without adjusting the diet and cooking methods. With the disease, the inflamed mucous membrane of the tonsils is sensitive to temperature changes. Moreover, not only cold drinks, but also hot drinks can cause damage: cold drinks increase inflammation, hot drinks burn the inflamed mucous membrane and lead to increased swelling. Food and drink should be warm enough, but not hot.
Food should be gentle not only thermally, but also mechanically and chemically. This means that in the acute period it can only be soft, crushed or pureed, not very salty and not spicy. You can drink non-concentrated broths. Mashed potatoes and boiled eggs are good for the body.
A sore throat during breastfeeding will go away faster if loved ones can take care of the child and provide the woman with bed rest in the first few days of the illness. The room where the sick woman is located should be regularly ventilated. It is also necessary to carry out wet cleaning every day.
Treatment of a disease such as tonsillitis requires a nursing mother to scrupulously follow the doctor’s recommendations and take her condition seriously. It is very important not to be lazy and gargle as often as possible, not limiting yourself to aerosols and lozenges.
Is sore throat dangerous for babies?
Sore throat that occurs during breastfeeding is not an indication for stopping lactation. If a nursing mother gets sick, then specific antibodies enter the breast milk, which, when they reach the baby’s body, help the baby not to become infected or to suffer the disease much easier. Still, you should not neglect precautions: you must avoid sharing utensils, wear a mask, and wash your hands thoroughly. If possible, it is better to entrust the care of the baby to close people. This will help the woman not only protect the baby, but also devote more time to rest and recuperation.
The length of the incubation period depends on a number of factors. In adult patients, this stage of the disease lasts from 1 to 14 days. During this period, there is a possibility that the disease will be transmitted to the baby from the mother during breastfeeding.