Factors provoking the appearance of the disease
The appearance of hyperplastic rhinitis as an independent disease is observed very rarely. In most cases, the provoking factor is inflammation.
The causes of provocateurs are:
- unfavorable climatic features of the region;
- work in hazardous industries or in places with a high content of fine dust;
- hypothermia of the body;
- tendency to allergic reactions;
- pathological processes in the nasopharynx;
- smoking;
- disorders of the nervous system.
Under the influence of these factors, thickening of the nasal mucous tissue occurs. As a result, blood microcirculation in the nasal vessels is disrupted. As a result of emerging pathological processes, hyperplastic rhinitis intensifies.
Sinusitis
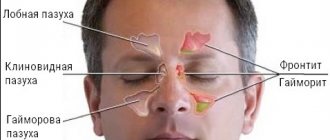
The nasal cavity communicates with seven paranasal sinuses: two frontal, two maxillary, two ethmoid and one sphenoid. The sinuses are connected to the nasal cavity by narrow passages. Through these passages, constant drainage (cleaning) of the sinuses is carried out. If the sinuses for some reason stop clearing, secretions stagnate in them and favorable conditions are created for the development of sinusitis.
The openings of the nasal sinuses can be blocked due to various deformations of the intranasal structures (hypertrophic rhinitis, curvature of the nasal septum, abnormalities in the structure of the ethmoid labyrinth and nasal concha). Viral infection is another risk factor for sinusitis. As a result of inflammation, the mucous membrane of the paranasal sinuses and nasal cavity swells. The mucous glands begin to produce large amounts of secretion. The openings of the paranasal sinuses narrow further due to swelling of the mucous membrane and become clogged with thick pathological secretions.
Impaired ventilation, stagnation of secretions and oxygen deficiency in the tissues of the sinuses become the impetus for the intensive development of opportunistic flora. A viral infection is accompanied by a bacterial one. The severity of sinusitis depends on the virulence of the microbes that cause inflammation. The widespread use of antibiotics leads to the fact that the bacterial flora that causes the development of sinusitis is often characterized by increased resistance (resistance) to most antibiotics.
In recent years, sinusitis is increasingly caused by fungi. The reason for this trend also lies in the unjustified use of antibiotic therapy, which negatively affects the state of the immune system, disrupts the normal composition of the microflora and creates favorable conditions for the development of mycotic infections. Sinusitis at the initial stage is not necessarily caused by microbes. Swelling of the mucous membrane, leading to the closure of the anastomosis of the paranasal sinuses, can be caused by inhalation of cold air and a number of chemicals.
However, the most common cause of sinusitis is immunodeficiency conditions and allergic reactions. Allergies cause vasomotor rhinitis, one of the manifestations of which is swelling of the nasal mucosa. The process is repeated several times. As a result, chronic sinusitis develops in approximately 80% of patients with vasomotor rhinitis.
Clinical picture of manifestation
In the early stages, the disease is characterized as an acute runny nose. As it develops, patients develop a number of symptoms characteristic of the hyperplastic form.
Rhinitis is accompanied by:
- difficulty breathing through the nose;
- prolonged snoring during sleep;
- dry mouth;
- loss of appetite;
- memory impairment;
- discomfort in the nasal passages;
- impaired sense of smell;
- nosebleeds;
- hearing impairment;
- mucous discharge from the nose;
- sore throat.
The disease in its later stages is accompanied by the development of a bacterial infection, a general deterioration in well-being and a weakening of the body’s protective functions.
Diagnosis of the disease
Rhinitis is diagnosed by an otolaryngologist. The diagnosis is made based on the collection of medical history and examination of the patient’s complaints. In addition to a visual examination, the doctor prescribes:
- blood for analysis;
- a swab from the nasal cavity to determine pathogenic microflora;
- endoscopic examination;
- diaphanoscopy;
- performing radiography;
- anemization test.
Hyperplastic rhinitis is diagnosed when studies show:
- blanching of the membranes of the nose;
- the presence of spots or areas of unusual color on the internal tissues of the nasal cavity;
- edema;
- infectious discharge;
- proliferation of nasal membrane cells;
- retraction of sections of the nasal passages into the nasopharynx area.
When diagnosing rhinitis, sinusitis, deformation of the nasal septum, and adenoids are often detected.
General principles of treatment
Hyperplastic rhinitis requires careful treatment. Based on the complexity of the disease, treatment is divided into physiotherapy and medication.
Therapeutic methods show high effectiveness only in the early stages, when hyperplasia is not clearly expressed.
Drug treatment consists of using:
- glucocorticosteroid drugs in the form of sprays (Avamys, Nasonex);
- injections of hormonal drugs, glucose, glycerin;
- silver-based drugs (Protargol, Collargol).
See also
Reasons why a child may grunt but there is no snot and what to do
Read
Conservative treatment is aimed at reducing areas of overgrown tissue and eliminating the inflammatory process.
If there is no result from the use of medications, physiotherapeutic treatment is used with cauterization of the overgrown areas. Physiotherapy is carried out in several stages.
- Inflamed areas are cauterized with chromic acid, laser or cryotherapy.
- In parallel, solutions and ointments are used aimed at reducing foci of inflammation (Collargol, Protargol).
- Ultrasound is applied to the affected areas.
For the most severe cases of hyperplastic rhinitis, surgical intervention is used. It is aimed at removing overgrown areas of soft tissue. The operation is called conchotomy. It involves excision of the hyperplasia zone with scissors or a loop.
Surgery and conservative treatment are not radical methods of treatment. Rhinosinusitis and its hyperplastic form can recur in the presence of provoking factors.
Myths and dangerous misconceptions about treating sinusitis
There is an opinion that sinusitis is a minor disease that will end in a week without treatment. However, it is worth remembering: the nasal sinuses are located close to the brain and eyes, to which the inflammatory process can spread under unfavorable circumstances. It should also be borne in mind that sometimes the natural opening connecting the cavities of the sinuses and nose is blocked, then there is no discharge at all. In this case, puncture and x-rays are used for diagnosis.
Another myth is related to punctures. They say that after one puncture you will have to do this procedure constantly. But today this is done quickly and painlessly, under local anesthesia. The puncture site heals without changing the anatomy of the sinus.
Possible complications
Lack of timely treatment leads to progression of the disease and the development of a number of complications.
The most common complications that arise are:
- nosebleeds;
- chronic inflammatory process in the nasopharynx;
- loss of smell;
- partial or complete hearing loss;
- headache.
As a result of untreated rhinitis and its chronic form, bronchitis, sinusitis, sinusitis, and conjunctivitis. In childhood, the main complication is chronic adenoiditis.
Experts also note disruption of the cardiovascular system, liver, and kidneys. The patient’s general well-being deteriorates, rapid fatigue, loss of appetite, and decreased performance appear.
Types and forms of exudative sinusitis
The classification of the disease, used to facilitate the choice of adequate therapy, is based on the mechanism of development of ES, so it is first of all important for a specialist to determine the nature of the inflammation. Here we distinguish between acute exudative sinusitis, which arose as a primary disease, and chronic, constantly recurrent. With acute damage to one or more paranasal sinuses and adequate treatment, the disease usually lasts no more than three weeks.
When a person makes mistakes in the treatment course prescribed to him, or simply ignores it, chronic exudative sinusitis develops. This form of the disease, although it does not have specific negative symptoms during the period of remission, is dangerous because it cannot be completely cured and often leads to serious complications.
Also, the classification of exudative type sinusitis has a direct connection with the stages of the disease.
Experts note the following sequence of development of the disease of this form:
- Catarrhal. The pathological process is characterized by the appearance of serous exudate in the paranasal sinuses. A disease of this type is considered the easiest to cure, but if errors are made in treatment measures, the disease actively progresses and in a short time passes into the next, more severe stage.
- Purulent. The most severe form of the pathological condition. With it, the exudate that accumulates in the sinuses becomes purulent in nature, which brings with it big problems with human health. The development of this type of disease is facilitated by the addition of bacterial flora to the infectious process.
- Hemorrhagic. This form of the disease is diagnosed quite rarely, but it brings no less negative consequences than the purulent form. Hemorrhagic sinusitis is especially dangerous in children, since for their fragile bodies, blood loss and the possible penetration of pathogenic microorganisms through the bloodstream from the paranasal sinuses into the brain pose a direct threat of developing serious, often irreversible consequences.
This classification of a pathological condition is necessary in medical practice for the most correct selection of therapeutic measures, allowing to eliminate the disease completely or transfer it to a state of long-term remission. Particular attention is paid to it when sinusitis is detected in pregnant women, since in this case the disease threatens the health and life of not only the woman, but also the unborn child. That is why otolaryngologists recommend that expectant mothers be more attentive to their health and, when the first negative symptoms appear, immediately seek advice from a specialist.
Hyperplastic sinusitis and its features
Hyperplastic sinusitis is rhinitis, in which inflammation of the mucous tissues of the nose develops with their subsequent transformation. The hyperplastic form is a subtype of productive sinusitis. It is associated with thickening of the tissues of the nose, causing difficulty breathing.
Rhinosinusitis is characterized by the appearance of symptoms such as:
- pain in the upper face and head;
- nasal discharge (color may vary depending on the stage of the disease and the cause of its appearance);
- impaired sense of smell;
- difficulty breathing;
- redness of the skin in the area of the affected sinus.
Rhinosinusitis is a general concept. It is divided into types depending on the infection that caused the inflammatory process and the location of the inflammation.
According to the type of infection, experts distinguish sinusitis:
- viral;
- allergic;
- bacterial;
- fungal;
- traumatic.
Depending on the location of the foci of inflammation, rhinosinusitis is divided into sinusitis, frontal sinusitis, ethmoiditis, and sphenoiditis.
See also
Review of the best nasal drops for chronic rhinitis
Read
Rhinosinusitis requires timely treatment. For this, antihistamines, drops with a vasoconstrictor effect, local antibiotics or hormones are used. Physiotherapy procedures have shown high effectiveness.
What is it[edit]
My face hurts. Sinusitis, sinusitis. Even such bullshit as a runny nose has complications, and they can be quite serious, so if a runny nose/cold is accompanied by pain under the eyes, above the bridge of the nose, or closer to the ears, it’s time to take a number to the doctor. Some time before this, snot of an unusual rainbow (yellow-green) color may appear - it would be nice to see an ENT specialist even then, but no matter what.
Due to the fact that all the organs in the head are located very close to each other, anything can leak from a sick face - even eye damage or meningitis, so our warm advice is not to delay such things, much less try to stay at home. Meningitis is very difficult to treat and can even lead to death.
Predisposition to rhinosinusitis is determined by smoking, allergic rhinitis, asthma, nasal polyps, hypersensitivity to aspirin, cystic fibrosis, and immunodeficiency. Secondary bacterial sinusitis is largely associated with preexisting respiratory diseases. An important factor in the disease leading to secondary bacterial sinusitis is obstruction of the ostiomeatal complex.
Pathogens of bacterial sinusitis[edit]
The main pathogens of bacterial sinusitis are pneumococcus (Streptococcus pneumoniae) and Haemophilus influenzae. Other microorganisms - pathogens include Moraxella catarrhalis and other streptococcal species (for example, Streptococcus pyogenes), Staphylococcus aureus (Staphylococcus aureus), anaerobic microorganisms (for example, Prevotella, Peptostreptococcus, Fusobacterium).
Pneumococcus is characterized by the greatest virulence and prevalence. Haemophilus influenzae can quickly spread throughout the nasopharynx. The microorganism is transmitted by airborne droplets or through direct contact with the secretions of an infected person.
Sinusitis is a common infection in intensive care units. The use of an endotracheal or gastric tube through the nose can cause inflammation of the nasopharyngeal mucosa, causing swelling in the area of the ostiomeatal complex. Also, the nasal tube can directly obstruct sinus drainage. Placing a tube in the mouth does not eliminate the risk of hospital-acquired sinusitis, but it does significantly reduce it. Another factor contributing to sinusitis is the supine position of patients, limited head movement (which impedes the natural drainage of the sinuses caused by gravity). Other factors for hospital-acquired sinusitis include forced-air ventilation, decreased ability to cough and sneeze, and lack of air flow through the nostrils in patients receiving mechanical ventilation.
Hyperplastic sinusitis and its features
Hyperplastic sinusitis is a type of sinusitis. It is characterized by the proliferation of mucous membranes in the maxillary sinuses. Sinusitis can be caused by allergic rhinosinusitis or an acute virus.
The pathology differs from other forms of rhinitis in a number of symptoms:
- swelling of the nose;
- impaired sense of smell;
- temperature up to 39 degrees;
- headache localized on the back of the head, frontal lobes, upper jaws;
- general weakness;
- purulent discharge from the nasal passages.
Based on localization, there are three forms of sinusitis.
- Right-handed. The pathological process affects only the right section of the nose.
- Left-handed. Overgrowth of mucous tissue, cystic and polypous formations appear on the left side.
- Bilateral. The most severe form, in which inflammation affects the maxillary sinuses on both sides.
The main treatment for the hyperplastic form of sinusitis is conservative. It is aimed at relieving the inflammatory process. Patients are prescribed broad-spectrum antibiotics. Swelling of the nasal tissues is eliminated through the use of vasoconstrictors and antihistamines.
To remove purulent contents from the nasal sinuses, they are washed with a solution of furatsilin or analogues. For treatment, drops on a hormonal basis or with a local antibiotic are used. Polydexa and Isofra have shown high effectiveness.
The absence of a visible effect from drug treatment is a reason for surgical intervention. It is aimed at removing overgrown tissue.
Prevention of acute sinusitis
Prevention of relapses of acute sinusitis requires compliance with the following preventive measures:
- Elimination of any existing anatomical defects if they interfere with the natural passage of air through the nasal passages;
- Dental treatment of tooth roots adjacent to the bottom of the maxillary sinus;
- Strengthening local and general immunity of the body.
The introduction of bacterial vaccines is also effective, allowing the population to be immunized.
Modern otolaryngologists are increasingly using the drug IRS-19. It contains lysates that fight bacterial agents that provoke ARVI. The product is available in the form of a spray and is aimed at activating the specific and nonspecific immunity of the mucous membrane of the ENT organs. Available clinical studies indicate that the drug reduces the number of relapses of sinusitis and other respiratory diseases by 2.5-4 times. To achieve maximum effect, it is advisable to carry out double immunization with a break of 4-5 months.
In addition, probiotics, for example, Normoflorin B and L, Laktofiltrum, have a preventive and therapeutic effect. They must be used both during treatment with antibacterial drugs and after the therapeutic course. At the same time, the state of the patient’s intestinal microflora should be monitored.
It is possible that aromatherapy can be used to prevent disease. The most commonly used aromatic oils are tea tree, mint, lavender, eucalyptus, etc. You can also use mixtures based on oils, for example, Citrosept, Carmolis, Eka, etc. They have a local vasoconstrictor effect, have a positive effect on nerve endings, relieve inflammation and fight with viruses.
Preventive actions
Preventive methods boil down to timely treatment of acute rhinitis and prevention of the development of the hyperplastic form. For prevention, you should follow several rules.
- Sanitation of the nasopharynx. Sanitation of the nasal passages and throat should be performed daily. The procedure is aimed at preventing the proliferation of mucous tissues and eliminating foci of infection.
- Consultation with an otolaryngologist. It is necessary to regularly visit an ENT doctor to monitor the dynamics of the process and timely prescribe treatment.
- Treatment of allergic reactions. It is important to exclude allergens from the diet and immediate environment, and to carry out preventive therapy during the flowering season.
- Strengthening the immune system. Activities include playing sports, giving up bad habits, switching to a healthy diet, and regular long walks in the fresh air.
Timely treatment of acute rhinitis avoids its progression and transition to a hyperplastic form.