General information
Nasal polyps (syn. polypous rhinosinusitis) are benign limited growths of hypertrophied/inflamed mucous membrane of the paranasal sinuses/nasal cavity, characterized by recurrent growth.
Polyps can be either single or multiple. The term “polyposis” is usually used when there are more than 10-20 polyps. Polypous rhinosinusitis (PRS) is a fairly common occurrence at any age, especially in individuals with chronic runny nose , chronic sinusitis , bronchial asthma , hay fever and intolerance to NSAIDs. The prevalence of PRS in the Russian Federation varies from 1 to 5%.
It was noted that the disease is more common in men than in women (2.2:1), mainly in patients over 30 years of age with a pronounced predominance in people in the age group of 50-60 years (average age 42 years). Nasal polyps in children and adolescents (under 20 years of age) are relatively rare. This disease is characterized by a severe course and a high relapse rate.
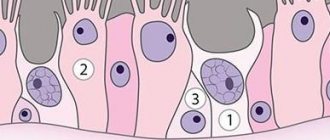
Histologically, the nasal polyp consists of damaged, often metaplastic epithelium located on a thickened basal membrane/edematous stroma, which contains a small number of glands and vessels, and there are practically no nerve endings. The stroma of the polyp contains fibroblasts, which form its supporting frame, as well as pseudocysts and cellular elements, among which eosinophils predominate, located directly under the surface epithelium and around the glands/vessels.
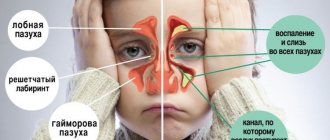
The formation of nasal polyps is caused by hypertrophy (excessive growth) of the nasal mucosa, which most often occurs as a result of a long-term inflammatory process. Hypertrophy of the nasal mucosa is considered as a compensatory mechanism for the inflammatory process in the nasal mucosa/sinuses, leading to an increase in the area of the mucosa, which leads to the formation of polyps. Most often, polyps develop from the maxillary/sphenoid sinuses, cells of the ethmoidal labyrinth, in the middle meatus/superior and middle turbinates; on the lateral wall of the nose. There are both solitary polyps, when one sinus is affected, and diffuse bilateral PRS, which is characterized by progressive damage to all SNPs/nasal cavity.
A separate nosological form is the choanal polyp (fibroma of the nasopharyngeal tract), which, despite certain similarities with the clinical picture of polypous rhinosinusitis/morphological structure of the formation, has different etio/pathogenetic mechanisms of development. The appearance of this type of polyp in the nasal sinuses is facilitated by various variants of abnormal development of the medial wall of the maxillary sinus. Developmental processes in the posterior nasal cavity also play a role, contributing to changes in the aerodynamics of the nasal cavity and the formation of single/multiple additional anastomosis in the posterior fontanella (photo on the right).
Choanal polyp is a rare pathology, the proportion of which does not exceed 4-6% of the number of various polypous rhinosinusitis and is more common in children. Based on the formation of the stalk of polyps in various anatomical structures, two types of choanal polyps can be distinguished: antrochoanal (polyp of the maxillary sinus) and sphenochoanal (growing from the sphenoid sinus).
Causes of hypertrophic rhinitis
Hypertrophic rhinitis is a disease that has many causative factors that cause it. The main ones are listed below.
1. Acute respiratory diseases (including ARVI). Frequently recurring infectious viral diseases in their acute phase lead to the formation of immune complexes in the blood and the activation of specific antibodies. The main consequence of the increased functioning of the immune system is an increase in the functioning of the nasal secretory apparatus and the production of large amounts of mucus, as well as thickening and proliferation of the mucous membrane. This pathology is caused by frequent exacerbations of acute respiratory diseases, on average five or more per year.
2. Deviation of the nasal septum. This anatomical pathology of the appearance of hypertrophy of the nasal mucosa causes narrowing of the nasal passages and difficulty in the normal outflow of mucus. Impaired capillary circulation and hypoxia of cells of the nasal mucosa include a mechanism for increased cell growth to compensate for these phenomena. Hence - hypertrophic rhinitis.
3. Congenital or acquired anomalies in the development of the nasal passages. The pathogenesis (mechanism of development) of hypertrophic rhinitis in this case is identical to the previous case.
4. Injuries to the nasal bones. As a consequence of traumatic damage to the nasal bones and changes in the size of the nasal passages, a disturbance in the outflow of mucus and congestion may occur. As a consequence of the latter, hypertrophy of the nasal mucosa occurs.
5. Long-term use of vasoconstrictor drugs. Uncontrolled long-term use of nasal sprays or drops with a vasoconstrictor effect can also lead to disruption of the blood supply to the nasal mucosa and its growth through a compensatory mechanism. At the same time, the nasal mucosa thickens, its vessels become fragile, and frequent nosebleeds appear.
6. External irritating factors. Most often these are environmental factors, work in hazardous industries, temperature factors (low or high air temperature), inhalation of dust or gases. All these factors can cause irritation of the nasal mucosa and, as a result, cause inflammation. Chronic exposure and inflammation of the mucous membrane leads to its degeneration and thickening. Inhalation of dust over a long period causes damage to the ciliated epithelium, which leads to the development of metaplasia and a slowdown in the outflow of secretions, as well as the formation of rhinoliths (nasal stones).
7. Cardiovascular pathology. Atherosclerosis of blood vessels (narrowing of their lumen) and hypertension are one of the causes of impaired blood supply to the nasal mucosa, tissue hypoxia and their hyperplastic degeneration.
8. Nasal infections. Polyps, cysts, and adenoids are a reservoir for the proliferation of many types of bacteria and viruses. The latter always cause inflammation of the nasal mucosa, and repeated episodes of inflammation lead to overgrowth of the mucous membrane.
Pathogenesis
The pathogenetic mechanisms of the formation and development of nasal polyps are widely discussed and not fully understood. According to many authors, the pathogenesis is based on the chronic inflammatory process (eosinophilic inflammation), which contributes to a qualitative change in the glycoproteins of the basement membrane, as well as vasodilation, exudation, deposits and fibrin organization.
An important role in the pathogenesis of the disease is assigned to the allergic component, that is, PRS is considered an infectious-allergic disease. Analysis of the literature data allows us to conclude that at least three types of allergic reactions are involved (I – reagin; III – immunocomplex; IV – delayed-type hypersensitivity).
Proponents of the autoimmune concept believe that the leading trigger for the autoallergic process is the direct effect on the mucous membrane of an infectious agent, which contributes to the development of chronic inflammation, as a result of which the nasal mucosa acquires the specific properties of the antigen. Accordingly, in response to the influence of complex antigens, which contain association products of microbial and tissue components, autoantibodies are synthesized in the body. The formation of immune complexes, in turn, leads to a cytotoxic effect on the mucous membrane of the paranasal sinuses/nasal cavity, causing its further changes. Thus, a cyclical process is formed, which becomes sluggish and long-term in nature with a high tendency to relapse.
There are other theories of the pathogenesis of the disease that suggest the participation of mechanical, constitutional and genetic factors in the etiopathogenesis of nasal polyposis. Thus, it is assumed that the development of nasal polyps is based on a local insufficiency of the mechanisms responsible for cleansing the nasal mucosa from inflammatory alteration products.
The gradual accumulation of such products contributes to long-term persistence of inflammation and increased local inflammatory edema with the development of a proliferative process and subsequent sclerosis of stromal elements. Such morphological changes in polyps lead to the development of lymphostasis, caused by dynamic insufficiency of the lymphatic bed; in an upright position, it helps to strengthen the “noose” mechanism in the anastomosis area. Also, according to a number of authors, the development of a local polypous process may be due to a violation of the aerodynamics of the nasal cavity due to anomalies/disturbances in the structure of the intranasal structures.
According to the theory of multifactoriality, various congenital/acquired biological defects can potentially exist in the human body at various levels (organ, cellular/subcellular), in particular, in the form of a pronounced imbalance of the autonomic nervous system, including hyperreactivity of the parasympathetic department. These defects can manifest clinically if there are provoking environmental factors (mechanical/physical/chemical influences, infectious agents or allergens) that act as a trigger. The severity of the reaction is determined by a number of factors: the virulence of the pathogen, local/general nonspecific and specific reactivity, the response of the autonomic nervous system, the nature of the dysfunction of the mucous membrane caused by obstacles (local malformations) in the path of mucociliary transport and elements of the mucous membrane (cilia immobility syndrome, etc. .), performing mucociliary transport.
Classification
There is no generally accepted classification of PRS. In routine clinical practice, it is customary to divide PRS based on possible etiological factors, features of the clinical course and the histological structure of the polyps.
According to the etio-pathogenetic principle, the following are distinguished:
- Polyposis caused by aerodynamic disturbances in the SNA/nasal cavity.
- Polyposis caused by chronic sluggish purulent inflammation of the mucous membrane of the SNP/nasal cavity.
- Polyposis caused by fungal infection of the mucous membrane of the SNP.
- Polyposis is based on disturbances in the metabolism of arachidonic acid .
- Polyposis in Kartagener syndrome/cystic fibrosis .
Based on the histological structure, they are distinguished:
- Fibroinflammatory polyps (neutrophilic).
- Edema, eosinophilic polyps.
- Glandular polyps.
- Polyps with atypical stroma.
According to endoscopic studies, several stages are distinguished that characterize the prevalence of the polyposis process:
- Stage 1 – it is characterized by persistent diffuse swelling of the mucous membrane localized in the middle nasal meatus.
- Stage 2 – polyps that are located in the middle nasal meatus and do not extend beyond its boundaries.
- Stage 2 - polyps already extend directly beyond the boundaries of the middle nasal meatus/localization of polypous changes in the mucous membrane on the medial surface of the nasal concha.
- Stage 4 – the presence of polyps in the common nasal passage.
According to the morphological classification, nasal polyps go through two stages of development: the stage of glandular-cystic (edematous) polyp and the stage of fibrous polyp.
Types of turbinate hypertrophy
The anatomical structure of the nasal passage and the movement of air currents leads to the fact that the most vulnerable places are the anterior end of the middle concha and the posterior end of the inferior concha. Most often, this is where hypertrophic changes occur. Therefore, hypertrophy of the nasal turbinates can be divided into the following types:
- hypertrophy of the posterior ends of the inferior turbinates - occurs quite often in people suffering from chronic rhinitis. The examination reveals formations in the form of polyps that cover the lumen of the internal nasal openings. Hypertrophy usually develops on both sides, but asymmetrically;
- hypertrophy of the anterior ends of the middle shells is determined less frequently. The cause of its occurrence is mainly sluggish inflammation of the accompanying sinus.
Causes
The causes of nasal polyps are not fully understood today. The main reasons include:
- Long-term, sluggish inflammation of the nasal cavity/sinuses ( sinusitis , chronic rhinitis , ethmoiditis ).
- Allergic diseases ( allergic rhinitis , bronchial asthma ), contributing to damage to the mucous membrane and its polypous degeneration.
- Hereditary factors ( cystic fibrosis , which is characterized by the accumulation of viscous secretions that cause inflammation in the sinuses and Kartagener syndrome with an autosomal recessive type of inheritance, in which the formation of polyps is caused by dysfunction of the motor cilia of the ciliated epithelium).
- Anatomical features/anomalies of the structure of the nose (deviated septum, narrowness of the nasal passages, anomalies of the middle turbinate, fissure in the nose) causing disturbances in the aerodynamics of the nasal cavity and contributing to the development of a local polypous process.
Symptoms of nasal polyps
Nasal polyps in adults manifest with patient complaints of persistent nasal congestion and varying degrees of difficulty in nasal breathing and snoring. Moreover, as the polyps grow, partial nasal congestion often turns into a complete blockage, which forces the patient to breathe through the mouth. The use of vasoconstrictor drops, as a rule, does not eliminate nasal congestion.
Long-term disruption of nasal breathing caused by nasal polyps leads to disorders of lymph/blood circulation in the brain area, which is manifested by increased fatigue, the appearance of headaches without a specific localization, decreased mental performance and sleep disturbances in patients. Most people with nasal polyps experience frequent sneezing/ running nose . Patients often complain of a deterioration in their sense of smell, including a complete inability to perceive smells ( anosmia ).
Some patients experience constant discomfort in the nose or a sensation of a foreign body. There may be pain in the various paranasal sinuses and thick nasal discharge (clumps of mucus). When polyps are localized in the posterior parts of the nasal cavity, a characteristic symptom is the appearance of nasal sounds (rhinolalia). What nasal polyps look like is shown below (photo of nasal polyps).
In general, the symptoms of nasal polyposis in adults and their severity are determined directly by the extent of the pathological process.
Treatment tactics
Treatment of hypertrophic rhinitis is aimed at eliminating the underlying cause, relieving symptoms, restoring mucous membranes and preventing exacerbations and progression of the disease.
Treatment methods at the initial stage of the disease
Conservative treatment is used only in mild and moderate stages of the pathological process. If the epithelium undergoes total deformation, then surgical intervention is necessary. The following treatment regimen is prescribed:
- Treatment of nostrils with Splenin ointment. The product contains a protein component, has a powerful antihistamine, regenerating and anti-edematous effect, and triggers a regenerative mechanism.
- Hydrocortisone injections (aka nasal blockade). Hormonal drugs relieve swelling, have an anti-inflammatory and regenerating effect, and normalize nasal breathing.
- Vasoconstrictor drugs. They relieve swelling, stimulate the activity of adrenergic receptors, and prevent further thickening of the mucous membranes. Naphazoline, Ephedrine, Xylometazoline, Phenylephrine are widely used.
Drug therapy is effective along with physiotherapy: UHF heating, laser therapy, electrophoresis with drugs, warming applications.
Surgical options
Surgical intervention is a radical method of getting rid of the symptoms of hypertrophic rhinitis and includes the following types of manipulations:
- conchotomy (partial, total or submucosal) - involves excision of the middle and lower part of the nasal concha, and if the periosteum is involved in the pathology - complete or partial removal of the nose along with elements of bone tissue (osteoconchotomy);
- cryodestruction – exposure of the affected area of the membranes to a special applicator with liquid nitrogen;
- laser vasotomy – coagulation of vessels of the submucosal membranes of the nasal passages;
- ultrasonic disintegration – ultrasonic sclerosis of the vessels of the nasal membranes.
After surgery, a rehabilitation period begins, which includes mandatory drug treatment, physiotherapy, and adherence to a protective regime.
Traditional methods
Non-traditional treatment methods are not used as monotherapy for chronic hypertrophic rhinitis. Efficacy has been confirmed only when used in combination with medications or after surgery. Popular recipes are:
- A decoction based on woodlice. 1 tbsp. plants are poured with 200 ml of boiling water, infused, filtered and the nasal passages are washed generously through a syringe without a needle 3-4 times a day.
- Decoction for rinsing based on chamomile, calendula, sage, plantain. 2 tbsp. dry plant mixture is poured with 500 ml of boiling water, cooled to room temperature, filtered and washed out the nose for 24 hours.
- Oil instillation. 5 drops of sea buckthorn, flaxseed, olive oil are mixed and instilled into the nasal passages 3-4 times a day. Place 4 drops in each nostril. The product helps with crusts, excessive dryness, and also with rhinorrhea.
Self-medication for hypertrophic rhinitis is unacceptable, as it can provoke the development of neoplasms, deep destruction of the nasal membranes and submucosal structures.
Tests and diagnostics
The diagnosis of diffuse and unilateral local PRS is made on the basis of patient complaints, medical history, examination and additional diagnostic methods. Objective methods include anterior/posterior rhinoscopy and, if necessary (polyps in hard-to-reach places), endoscopy of the nasal cavity. The leading role in the diagnosis of polyposis is given to computed tomography of the SNP, which makes it possible to establish the prevalence of the polyposis process, as well as determine the presence/severity of destruction of intranasal structures. If necessary, probing/puncture of the paranasal sinuses, skin tests with allergens and determination of eosinophils in the blood/nasal mucus are performed.
X-ray examination of the SNP is relatively uninformative. Magnetic resonance imaging does not have great diagnostic significance and is mainly used for differential diagnosis. In case of PRS on the background of bronchial asthma, it is necessary to study the function of external respiration. Differential diagnosis is carried out with cysts/neoplasms of the SNP and nasal cavity, fungal/chronic bacterial rhinosinusitis .
Diagnostics
Only an experienced ENT specialist can determine the presence of chronic pathology. The initial examination begins with collecting a pathological history. To establish a diagnosis, an X-ray of the sinuses is performed (in especially severe cases, MRI or CT).
If the diagnosis of chronic sinusitis is difficult, puncture of the maxillary sinuses is performed. It is often supplemented by rinsing with an antiseptic and introducing antibacterial agents. During the puncture, a smear is made to determine the nature of the flora. It is used for subsequent diagnostic measures, which make it possible to identify a specific pathogenic microorganism and determine its sensitivity to antibiotics. It is impossible to prescribe complete treatment without a complete examination.
Rhinoscopy is used quite often; a similar method is aimed at determining the condition of the mucous membrane. The otolaryngologist examines the patient using a nasal and nasopharyngeal speculum under artificial light.
It is interesting to know that in patients with hyperplastic sinusitis, a pronounced dark stripe is often detected on x-rays . Its outline has clear outlines. If polyps are present, the darkening may be uneven.
It is worth remembering that radiography is not an accurate enough method, and in some cases, to establish an accurate diagnosis, you need to resort to new techniques, such as CT and MRI.
In children
The appearance of nasal polyps in a child and the absence of normal nasal breathing leads to improper formation of the dental system, which is manifested by malocclusion and facial cranium disorders. Enlarged polyps are accompanied by a high risk of blocking the entrance from the nasopharynx to the auditory tube, which leads to decreased hearing (hearing loss) and impaired speech development of the child. Nasal polyps in children of the first year of life and difficulty breathing through the nose can cause disturbances in the process of sucking or swallowing food, which, in the absence of adequate treatment, leads to chronic malnutrition and the development of malnutrition. Treatment of children is not fundamentally different from adults, but drug therapy is carried out taking into account age.
Prevention
Prevention of nasal polyps comes down to timely detection of acute inflammatory processes in the nasopharynx (early diagnosis), provoking uncontrolled hyperplasia of the nasal mucosa , allergic diseases, prescribing correct/timely treatment, and preventing the transition of acute nasal diseases and SNP into a chronic form. It is also recommended to minimize contact with allergens in cases of allergies; do not use vasoconstrictor nasal drops for more than 5 days; if necessary, avoid taking NSAIDs; rinsing the nasal cavity twice with solutions of sea salt ( Aquamaris , Hummer , Quicks , etc.); maintaining immunity ; If persistent nasal congestion occurs, immediately contact a specialist.
Consequences and complications
Modern therapeutic/surgical methods for treating PRS do not guarantee the absence of recurrence of nasal polyps. In the absence of timely or inadequate treatment, there is a high risk of developing persistent anosmia, and the ability to perceive odors may not be restored even after surgical removal of polyps. Due to the obstruction of air through the nose by polyps, the patient is forced to partially/completely switch to breathing through the mouth, which leads to the entry of cold/dry air into the respiratory tract. That is, impaired nasal breathing with nasal polyps contributes to the development of laryngitis , pharyngitis , tracheitis , laryngotracheitis and bronchitis .
When polyps block the anastomoses of the paranasal sinuses, there is a risk of developing an inflammatory process (sinusitis) in them. With large polyps, blood vessels can be compressed, which also causes circulatory problems in the nasopharyngeal structures/tissues and is the cause of periodic inflammation of the palatine tonsils with the development of sore throat , pharyngeal tonsil with the development of chronic tonsillitis / adenoids , or inflammation of the middle ear ( otitis )/auditory tube ( eustachitis ).
Features of therapy
Treatment of right-sided or left-sided hyperplastic sinusitis is related to the cause that caused the development of the disease.
Methods:
- surgical;
- medicinal.
For treatment, a comprehensive treatment method is used to successfully cope with the symptoms of the disease.
The allergic nature of hyperplastic sinusitis involves taking antihistamines: Suprastin, Tavegil.
When the disease develops due to infection with pathogenic organisms, antibacterial drugs are prescribed: Amoxiclav, Flemoxin Solutab. It is important not to self-medicate, especially for children.
Additional therapeutic measures:
- washing the nasal cavity to remove mucous secretions using saline solutions, as well as carrying out inhalation procedures with Interferon, Chlorophyllipt;
- elimination of swelling of the sinuses with the help of drugs that constrict blood vessels: Tizin Xylo, Nazivin).
Particular attention is paid when prescribing therapy for hyperplastic sinusitis to a pregnant woman, since the composition of some medications can negatively affect the unborn child and the mother.
Surgical intervention takes place in the absence of a therapeutic effect from traditional treatment. Usually gentle operations are performed using an endoscope.
List of sources
- Piskunov G.Z. Polyposis of the nose and paranasal sinuses and its treatment / Russian rhinology. 2003; No. 2., p. 10-13.
- Ryazantsev S.V., Maryanovsky A.A. Polypous rhinosinusitis: etiology, pathogenesis, clinical picture and modern methods of treatment. Guidelines. St. Petersburg; 2006.
- Lopatin A.S. Modern theories of the pathogenesis of polypous rhinosinusitis // Pulmonology. –2003. – No. 5. – P. 110 – 115.
- Piskunov S.Z., Barsukov V.S., Zavyalov F.N., Piskunov I.S., Kuznetsova O.N. On the issue of pathogenesis and morphogenesis of antrochoanal polyps / Russian Rhinology. 1997; 3:22.
- Pukhlik S.M. Polypous rhinosinusitis. Clinical immunology, allergology, infectology // special issue, 2010. p. 5-10.